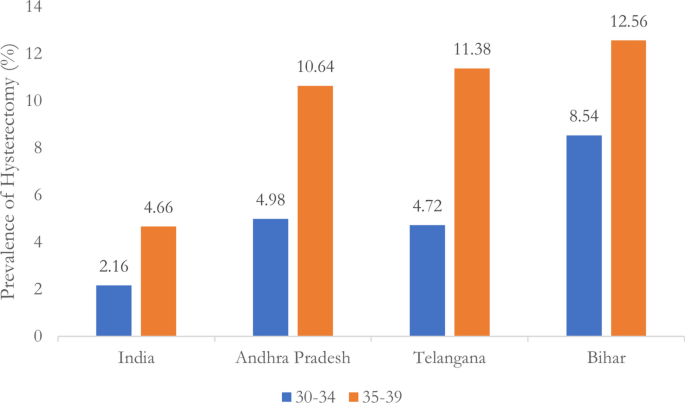
This study has revealed a concerningly high prevalence of premature menopause among women in Bihar, India. These findings demonstrate that Bihar’s rates of premature menopause exceed national averages and those of other high-prevalence states, even after accounting for the influence of hysterectomies. Regression analysis identified several key factors associated with premature menopause in Bihar, including lower education, younger age at first birth, and, most strikingly, female sterilization.
The most striking and concerning finding in this study is the strong association between female sterilization and both naturally induced and hysterectomy-induced premature menopause in Bihar. It is important to clarify the distinction between these two types of premature menopause. Naturally occurring premature menopause refers to the cessation of menstruation before age 40 due to natural causes. Hysterectomy-induced premature menopause occurs when a hysterectomy, particularly one involving the removal of both ovaries (oophorectomy), leads to the premature cessation of menstruation and ovarian hormone production. Our findings indicate that female sterilization is associated with both of these outcomes in Bihar.
It’s important to note that female sterilization itself (tubal ligation) does not directly interfere with ovarian function or hormone production. Therefore, the high prevalence of premature menopause among sterilized women in Bihar is unlikely to be a direct result of the sterilization procedure itself. However, the quality and safety of sterilization procedures in the region could be an indirect contributing factor. Botched sterilizations may lead to complications such as pelvic inflammatory disease, chronic pain, or excessive bleeding, which, in turn, could necessitate hysterectomies. If these hysterectomies involve the removal of the ovaries (oophorectomy), they would directly induce menopause. It’s essential to acknowledge that, due to data limitations, we were unable to determine the specific type of hysterectomy (with or without oophorectomy) performed on women in our sample, which limits our ability to precisely quantify the contribution of hysterectomy to premature menopause. To mitigate this, our analysis also focused on naturally occurring premature menopause, which is independent of hysterectomy.
Several potential explanations for this association, beyond the direct impact of the procedure itself, warrant further investigation. Previous studies in India have suggested a link between sterilization and an increased risk of hysterectomy14,15. The high rates of female sterilization, often perceived as a straightforward means of family planning once a desired family size is reached, may inadvertently contribute to later hysterectomy needs due to complications like Pelvic Inflammatory Disease or other gynecological issues14,16. The fact that this study found sterilization to be a significant predictor of both naturally induced menopause and hysterectomy in Bihar further underscores the need to investigate this complex interplay.
A critical consideration is the potential for selection bias. Women who choose sterilization may differ systematically from women who choose other contraceptive methods or no contraception at all. They may have a higher prevalence of pre-existing gynecological conditions, face greater socioeconomic pressures, or have different reproductive health preferences. While I controlled for several socioeconomic factors in the analysis, unmeasured confounders could still contribute to the observed association. For instance, women experiencing early perimenopausal symptoms, such as irregular bleeding, might be more inclined to choose sterilization as a permanent method of contraception. This potential for reverse causality complicates our ability to conclude that sterilization causes premature menopause.
Beyond the direct impact of the procedure itself, the quality and safety of sterilization procedures in Bihar could be an indirect contributing factor to premature menopause. News reports have conducted exposés on Bihar’s sterilization camps where poor women have been sterilized in exchange for monetary compensation17. These exposés highlight the coercive tactics used by health officials to get women amenable to sterilization and the deplorable conditions under which the sterilizations were performed17,18. For impoverished women from rural areas, sterilizations are typically conducted in outpatient, government sterilization camps in temporary facilities such as small schools and public health clinics19. The conditions of these camps have long been criticized by scholars for their unsafe and unsanitary conditions19,20. The potential for coercion and lack of informed consent in these settings raises serious ethical concerns. This can be seen as a violation of women’s reproductive rights and bodily autonomy. The observed association between sterilization and premature menopause may reflect the long-term consequences of these unethical practices and the neglect of women’s reproductive health needs.
To address these ethical concerns, several policy reforms are needed. First, stricter regulations and monitoring of sterilization camps are essential to ensure adherence to safety standards and ethical guidelines. Second, healthcare providers need comprehensive training on informed consent, counseling, and the provision of a full range of contraceptive options, empowering women to make voluntary and informed decisions about their reproductive health. Third, increased investment in public health infrastructure and access to quality healthcare services is crucial to reduce the reliance on sterilization as the primary method of family planning and to address the underlying health issues that may contribute to the need for hysterectomies.
While the finding between sterilization and premature menopause is correlational and does not establish a causal link, it raises serious concerns about the potential for coercion and lack of informed consent in family planning programs. Scholars have argued that population control policies often disproportionately target women from lower socioeconomic backgrounds21,22. This targeting can result in the neglect of their individual reproductive needs and rights.
Beyond sterilization, these findings highlight the persistent influence of social determinants of health on women’s reproductive health in Bihar. Lower education was consistently associated with a higher risk of premature menopause, underscoring the importance of investing in girls’ education and women’s empowerment. Interestingly, wealth was not a significant predictor of premature menopause in Bihar, despite its effect in other regions of India. This suggests that other factors, potentially specific to Bihar, may be overriding the benefits of socioeconomic advantage. These factors might include caste discrimination in healthcare access, cultural norms around women’s health, limited access to quality healthcare in rural areas. In other words, socioeconomic advantage alone may not be sufficient to mitigate premature menopause risk when women face systemic gender inequalities and limited access to quality healthcare.
Future research should adopt an intersectional feminist lens to examine how the interplay of gender, caste, class, and other social identities shapes the risk of premature menopause and access to reproductive healthcare in Bihar. For instance, lower-caste women in rural areas may face greater barriers to accessing quality reproductive healthcare, increasing their risk of complications and, ultimately, hysterectomy. This approach can provide a more nuanced understanding of the complex factors contributing to the state’s high premature menopause rates.
The association between younger age at first birth and increased premature menopause risk is consistent with a growing body of research highlighting the long-term health consequences of early childbearing23. This finding underscores the need for adolescent reproductive health programs and expanded access to family planning services in Bihar.
The results also point to potential concerns regarding the utilization of hysterectomies. The finding that health insurance coverage is a risk factor for hysterectomy in Bihar suggests that access to insurance may be driving increased utilization of this procedure, potentially due to financial incentives for providers or greater healthcare-seeking behavior among insured women. Another possibility is that women with insurance are more likely to be diagnosed with gynecological problems, leading to a higher rate of hysterectomies. This warrants further investigation to ensure that hysterectomies are being performed only when medically necessary.
The negative association between anemia and both naturally induced menopause and hysterectomy was an unexpected finding. While the reasons for this are unclear, one possible explanation is that women with severe anemia may be considered less suitable candidates for elective surgeries like hysterectomy. Alternatively, severe anemia might be associated with lighter or less frequent periods, which could delay the self-recognition or reporting of menopause. Further research is needed to fully understand the complex relationship between anemia and menopause in this population.
The findings from the study all for a comprehensive and multifaceted public health response tailored to the specific needs of women in Bihar. This response must move beyond a narrow focus on hysterectomy and address the broader social, economic, and reproductive health factors driving premature menopause in this region. Priority actions include increasing investments in girls’ education and women’s socioeconomic empowerment, expanding access to adolescent reproductive health programs, and promoting a wider range of family planning options beyond sterilization. Specifically, this includes mandatory training programs for healthcare providers, public health campaigns, strengthening monitoring and regulation of sterilization camps and increased access to quality reproductive healthcare.
Moving forward, one needs to critically examine the quality and safety of sterilization practices in Bihar. This requires implementing stricter regulations and monitoring of sterilization camps, investing in training and resources for healthcare providers to ensure safe and ethical sterilization procedures, and empowering women with information about the potential risks and benefits of different family planning methods. Raising awareness among women and healthcare providers about the risks and long-term consequences of premature menopause, including the potential role of sterilization, is vital for enabling women to make informed decisions about their reproductive health.
While the findings from this study offer valuable insights into the drivers of premature menopause in Bihar, it is essential to acknowledge the limitations of the study. First, the cross-sectional nature of the NFHS-5 data prevents us from establishing causal relationships between the identified risk factors and premature menopause. Longitudinal studies are needed to better understand the temporal relationships and causal pathways involved. Second, as with all survey data, self-reported information on menopause status and other variables is subject to recall bias and social desirability bias, which could influence the findings. Third, the NFHS-5 dataset does not provide detailed information on the types of hysterectomies performed (with or without oophorectomy) or the specific methods of female sterilization used, or the types of contraceptives used (hormonal, barrier, natural). This limitation prevents us from fully disentangling the potential mechanisms linking these procedures to premature menopause. Additionally, we were unable to explore the role of certain factors that have been linked to premature menopause in other studies, such as smoking, genetic predisposition, and environmental exposures, due to data limitations. Future research incorporating these variables and using more detailed data on sterilization procedures, hysterectomy types and contraceptive methods would provide a more comprehensive understanding of the complex drivers of premature menopause in Bihar.
link






