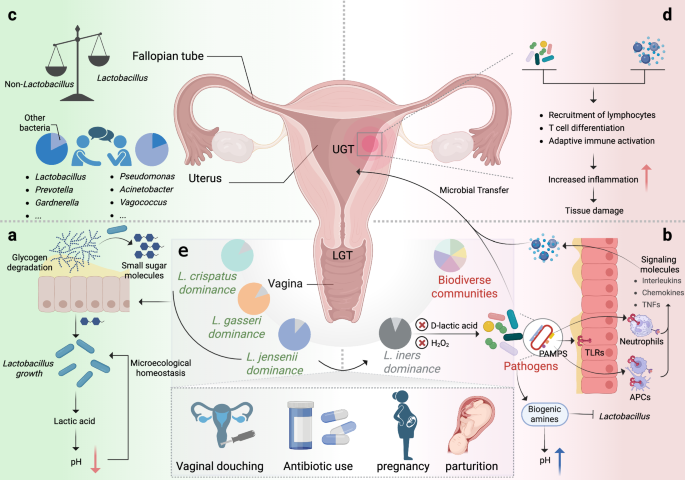
Condori-Catachura, S. et al. Diversity in women and their vaginal microbiota. Trends Microbiol. (2025).
Weinstein, L. The bacterial flora of the human vagina. Yale J. Biol. Med. 10, 247–260 (1938).
Google Scholar
Kampmeier, R. H. Identification of the gonococcus by Albert Neisser. Sex. Transm. Dis. 5, 71–72 (1978).
Google Scholar
Catlin, B. W. Gardnerella vaginalis: characteristics, clinical considerations, and controversies. Clin. Microbiol. Rev. 5, 213–237 (1992).
Google Scholar
O’Connor, B. H. Genital chlamydial infection. Br. Med J. 2, 771 (1978).
Google Scholar
Gnarpe, H. & Friberg, J. Mycoplasma and human reproductive failure: I. the occurrence of different Mycoplasmas in couples with reproductive failure. Am. J. Obstet. Gynecol. 114, 727–731 (1972).
Google Scholar
Love, W., Jones, M., Andrews, B. & Thomas, M. Mycoplasmas in human infertility. Lancet 1, 1130–1131 (1973).
Google Scholar
Barbés, C. & Boris, S. Potential role of lactobacilli as prophylactic agents against genital pathogens. Aids Patient Care STDS 13, 747–751 (1999).
Google Scholar
Rush, C. M., Hafner, L. M. & Timms, P. Genetic modification of a vaginal strain of Lactobacillus fermentum and its maintenance within the reproductive tract after intravaginal administration. J. Med. Microbiol. 41, 272–278 (1994).
Google Scholar
Spiegel, C. A. Bacterial vaginosis. Clin. Microbiol. Rev. 4, 485–502 (1991).
Google Scholar
consortium, I. H. i. r. n. The integrative human microbiome project. Nature 569, 641–648 (2019).
Google Scholar
Ravel, J. et al. Vaginal microbiome of reproductive-age women. Proc. Natl. Acad. Sci. USA 108, 4680–4687 (2011).
Google Scholar
consortium, T. H. M. P. Structure, function and diversity of the healthy human microbiome. Nature 486, 207–214 (2012).
Google Scholar
Chen, C. et al. The microbiota continuum along the female reproductive tract and its relation to uterine-related diseases. Nat. Commun. 8, 875 (2017).
Google Scholar
Walther-António, M. R. et al. Potential contribution of the uterine microbiome in the development of endometrial cancer. Genome Med. 8, 122 (2016).
Google Scholar
Moreno, I. et al. Evidence that the endometrial microbiota has an effect on implantation success or failure. Am. J. Obstet. Gynecol. 215, 684–703 (2016).
Google Scholar
Fettweis, J. M. et al. The vaginal microbiome and preterm birth. Nat. Med. 25, 1012–1021 (2019).
Google Scholar
Yefet, E. et al. Efficacy of oral probiotic supplementation in preventing vulvovaginal infections during pregnancy: a randomized and placebo-controlled clinical trial. Nutrients 16, (2024).
Koirala, R. et al. Effect of oral consumption of capsules containing Lactobacillus paracasei LPC-S01 on the vaginal microbiota of healthy adult women: a randomized, placebo-controlled, double-blind crossover study. FEMS Microbiol. Ecol. 96, (2020).
Menichini, D. et al. Probiotics in pregnancy and group B streptococcus colonization: a multicentric, randomized, placebo-controlled, double-blind study with a focus on vaginal microbioma. Eur. J. Obstet. Gynecol. Reprod. Biol. 310, 113976 (2025).
Google Scholar
Husain, S. et al. Effects of oral probiotic supplements on vaginal microbiota during pregnancy: a randomised, double-blind, placebo-controlled trial with microbiome analysis. Bjog 127, 275–284 (2020).
Google Scholar
Fu, M. et al. Alterations in vaginal microbiota and associated metabolome in women with recurrent implantation failure. mBio 11, e03242–19 (2020).
Google Scholar
Goldstein, E. J., Tyrrell, K. L. & Citron, D. M. Lactobacillus species: taxonomic complexity and controversial susceptibilities. Clin. Infect. Dis. 60, S98–S107 (2015).
Google Scholar
Łaniewski, P. & Herbst-Kralovetz, M. M. Connecting microbiome and menopause for healthy ageing. Nat. Microbiol. 7, 354–358 (2022).
Google Scholar
Miller, E. A., Beasley, D. E., Dunn, R. R. & Archie, E. A. Lactobacilli dominance and vaginal pH: why is the human vaginal microbiome unique?. Front. Microbiol. 7, 1936 (2016).
Google Scholar
Kwon, M. S. & Lee, H. K. Host and microbiome interplay shapes the vaginal microenvironment. Front. Immunol. 13, 919728 (2022).
Google Scholar
France, M., Alizadeh, M., Brown, S., Ma, B. & Ravel, J. Towards a deeper understanding of the vaginal microbiota. Nat. MICROBIOL 7, 367–378 (2022).
Google Scholar
Li, J., McCormick, J., Bocking, A. & Reid, G. Importance of vaginal microbes in reproductive health. Reprod. Sci. 19, 235–242 (2012).
Google Scholar
Petrova, M. I., Reid, G., Vaneechoutte, M. & Lebeer, S. Lactobacillus iners: friend or foe?. Trends Microbiol. 25, 182–191 (2017).
Google Scholar
Bloom, S. M. et al. Cysteine dependence of Lactobacillus iners is a potential therapeutic target for vaginal microbiota modulation. Nat. Microbiol. 7, 434–450 (2022).
Google Scholar
Bhattacharya, A., Das, S., Bhattacharjee, M. J., Mukherjee, A. K. & Khan, M. R. Comparative pangenomic analysis of predominant human vaginal lactobacilli strains towards population-specific adaptation: understanding the role in sustaining a balanced and healthy vaginal microenvironment. BMC Genomics 24, 565 (2023).
Google Scholar
Zhang, Q. et al. Comparative genomics of Lactobacillus crispatus from the gut and vagina reveals genetic diversity and lifestyle adaptation. Genes 11, 360 (2020).
Google Scholar
Huedo, P. et al. Whole-genome sequences of vaginal isolates Lactobacillus crispatus CECT30647 and Lactobacillus gasseri CECT30648. Microbiol. Resour. Announc. 13, e00794–00724 (2024).
Google Scholar
Zhang, J., Li, K., Cao, T. & Duan, Z. Characterization of a Lactobacillus gasseri strain as a probiotic for female vaginitis. Sci. Rep. 14, 14426 (2024).
Google Scholar
Macklaim, J. M., Gloor, G. B., Anukam, K. C., Cribby, S. & Reid, G. At the crossroads of vaginal health and disease, the genome sequence of Lactobacillus iners AB-1. Proc. Natl. Acad. Sci. USA 108, 4688–4695 (2011).
Google Scholar
Frese, S. A. et al. The evolution of host specialization in the vertebrate gut symbiont Lactobacillus reuteri. PLoS Genet. 7, e1001314 (2011).
Google Scholar
France, M. T., Mendes-Soares, H. & Forney, L. J. Genomic comparisons of Lactobacillus crispatus and Lactobacillus iners reveal potential ecological drivers of community composition in the vagina. Appl. Environ. Microbiol. 82, 7063–7073 (2016).
Google Scholar
Witkin, S. S. et al. Influence of vaginal bacteria and D- and L-lactic acid isomers on vaginal extracellular matrix metalloproteinase inducer: implications for protection against upper genital tract infections. mBio 4, (2013).
Gajer, P. et al. Temporal dynamics of the human vaginal microbiota. Sci. Transl. Med. 4, 132ra152 (2012).
Google Scholar
Munoz, A. et al. Modeling the temporal dynamics of cervicovaginal microbiota identifies targets that may promote reproductive health. Microbiome 9, 163 (2021).
Google Scholar
Onderdonk, A. B., Delaney, M. L. & Fichorova, R. N. The human microbiome during bacterial vaginosis. Clin. Microbiol. Rev. 29, 223–238 (2016).
Google Scholar
Neal, C. M., Kus, L. H., Eckert, L. O. & Peipert, J. F. Noncandidal vaginitis: a comprehensive approach to diagnosis and management. Am. J. Obstet. Gynecol. 222, 114–122 (2020).
Google Scholar
Yu, T. et al. Characteristics of the vaginal microbiota and vaginal metabolites in women with cervical dysplasia. Front. Cell. Infect. Microbiol. 14, 1457216 (2024).
Google Scholar
Ilhan, Z. E. et al. Deciphering the complex interplay between microbiota, HPV, inflammation and cancer through cervicovaginal metabolic profiling. EBioMedicine 44, 675–690 (2019).
Google Scholar
Lacroix, G., Gouyer, V., Gottrand, F. & Desseyn, J. L. The cervicovaginal mucus barrier. Int. J. Mol. Sci. 21, (2020).
Srinivasan, S. et al. Metabolic signatures of bacterial vaginosis. mBio 6, (2015).
Vitali, B. et al. Vaginal microbiome and metabolome highlight specific signatures of bacterial vaginosis. Eur. J. Clin. Microbiol. Infect. Dis. 34, 2367–2376 (2015).
Google Scholar
Laghi, L. et al. Rifaximin modulates the vaginal microbiome and metabolome in women affected by bacterial vaginosis. Antimicrob. Agents Chemother. 58, 3411–3420 (2014).
Google Scholar
Challa, A. et al. Multi-omics analysis identifies potential microbial and metabolite diagnostic biomarkers of bacterial vaginosis. J. Eur. Acad. Dermatol. Venereol. 38, 1152–1165 (2024).
Google Scholar
Yeoman, C. J. et al. A multi-omic systems-based approach reveals metabolic markers of bacterial vaginosis and insight into the disease. PLoS ONE 8, e56111 (2013).
Google Scholar
Nelson, T. M. et al. Vaginal biogenic amines: biomarkers of bacterial vaginosis or precursors to vaginal dysbiosis?. Front. Physiol. 6, 253 (2015).
Google Scholar
Borgogna, J. C. et al. Biogenic amines increase the odds of bacterial vaginosis and affect the growth of and lactic acid production by vaginal Lactobacillus spp. Appl. Environ. Microbiol. 87, (2021).
Roberton, A. M. et al. A novel bacterial mucinase, glycosulfatase, is associated with bacterial vaginosis. J. Clin. Microbiol. 43, 5504–5508 (2005).
Google Scholar
Doerflinger, S. Y., Throop, A. L. & Herbst-Kralovetz, M. M. Bacteria in the vaginal microbiome alter the innate immune response and barrier properties of the human vaginal epithelia in a species-specific manner. J. Infect. Dis. 209, 1989–1999 (2014).
Google Scholar
Lim, K. H. & Staudt, L. M. Toll-like receptor signaling. Cold Spring Harb. Perspect. Biol. 5, a011247 (2013).
Google Scholar
Wira, C. R., Fahey, J. V., Sentman, C. L., Pioli, P. A. & Shen, L. Innate and adaptive immunity in female genital tract: cellular responses and interactions. Immunol. Rev. 206, 306–335 (2005).
Google Scholar
Park, B. S. & Lee, J. O. Recognition of lipopolysaccharide pattern by TLR4 complexes. Exp. Mol. Med. 45, e66 (2013).
Google Scholar
Chilton, P. M., Embry, C. A. & Mitchell, T. C. Effects of differences in lipid a structure on TLR4 pro-inflammatory signaling and inflammasome activation. Front. Immunol. 3, 154 (2012).
Google Scholar
Anahtar, M. N. et al. Cervicovaginal bacteria are a major modulator of host inflammatory responses in the female genital tract. Immunity 42, 965–976 (2015).
Google Scholar
Xiao, L., Zuo, Z. & Zhao, F. Microbiome in female reproductive health: implications for fertility and assisted reproductive technologies. Genom. Proteom. Bioinform. 22, (2024).
France, M. T. et al. VALENCIA: a nearest centroid classification method for vaginal microbial communities based on composition. Microbiome 8, 166 (2020).
Google Scholar
Mehta, S. D. et al. Host genetic factors associated with vaginal microbiome composition in Kenyan women. mSystems 5, (2020).
Murphy, K. et al. Genetic predictors for bacterial vaginosis in women living with and at risk for HIV infection. Am. J. Reprod. Immunol. 91, e13845 (2024).
Google Scholar
Mutli, E. et al. Genome-wide association study in Estonia reveals importance of vaginal epithelium associated genes in case of recurrent vaginitis. J. Reprod. Immunol. 162, 104216 (2024).
Google Scholar
Luo, Y. et al. A high-resolution HLA reference panel capturing global population diversity enables multi-ancestry fine-mapping in HIV host response. Nat. Genet. 53, 1504–1516 (2021).
Google Scholar
Kudela, E. et al. The interplay between the vaginal microbiome and innate immunity in the focus of predictive, preventive, and personalized medical approach to combat HPV-induced cervical cancer. EPMA J. 12, 199–220 (2021).
Google Scholar
Medhasi, S. & Chantratita, N. Human leukocyte antigen (HLA) system: genetics and association with bacterial and viral infections. J. Immunol. Res. 2022, 9710376 (2022).
Google Scholar
Arnaiz-Villena, A. et al. Complex interactions between the human major histocompatibility complex (MHC) and microbiota: their roles in disease pathogenesis and immune system regulation. Biomedicines 12, (2024).
Kubinak, J. L. et al. MHC variation sculpts individualized microbial communities that control susceptibility to enteric infection. Nat. Commun. 6, 8642 (2015).
Google Scholar
Mackelprang, R. D. et al. Toll-like receptor gene variants and bacterial vaginosis among HIV-1 infected and uninfected African women. Genes Immun. 16, 362–365 (2015).
Google Scholar
Taylor, B. D. et al. Toll-like receptor variants and cervical Atopobium vaginae infection in women with pelvic inflammatory disease. Am. J. Reprod. Immunol. 79, e12804 (2018).
Google Scholar
Si, J., You, H. J., Yu, J., Sung, J. & Ko, G. Prevotella as a hub for vaginal microbiota under the influence of host genetics and their association with obesity. Cell Host Microbe 21, 97–105 (2017).
Google Scholar
Taylor, B. D. et al. Cross-sectional analysis of Toll-like receptor variants and bacterial vaginosis in African–American women with pelvic inflammatory disease. Sex. Transm. Infect. 90, 563–566 (2014).
Google Scholar
Hugerth, L. W. et al. Defining vaginal community dynamics: daily microbiome transitions, the role of menstruation, bacteriophages, and bacterial genes. Microbiome 12, 153 (2024).
Google Scholar
Chee, W. J. Y., Chew, S. Y. & Than, L. T. L. Vaginal microbiota and the potential of Lactobacillus derivatives in maintaining vaginal health. Microb. Cell. Fact. 19, 203 (2020).
Google Scholar
Zhang, X. et al. Variation of the vaginal microbiome during and after pregnancy in Chinese women. Genom. Proteom. Bioinforma. 20, 322–333 (2022).
Google Scholar
Cao, W. et al. The effect of the female genital tract and gut microbiome on reproductive dysfunction. BioSci. Trends 17, 458–474 (2024).
Google Scholar
Liang, Y. et al. Highlight signatures of vaginal microbiota and metabolome contributed to the occurrence and recurrence of vulvovaginal candidiasis. Microbiol. Spectr. 12, e0152124 (2024).
Google Scholar
Chen, X. et al. Vaginal homeostasis features of Vulvovaginal Candidiasis through vaginal metabolic profiling. Med. Mycol. 61, (2023).
Song, J. et al. Interpretation of vaginal metagenomic characteristics in different types of vaginitis. mSystems 9, e0137723 (2024).
Google Scholar
Ceccarani, C. et al. Diversity of vaginal microbiome and metabolome during genital infections. Sci. Rep. 9, 14095 (2019).
Google Scholar
Norenhag, J. et al. Compositional and functional differences of the vaginal microbiota of women with and without cervical dysplasia. Sci. Rep. 14, 11183 (2024).
Google Scholar
Zhu, M. et al. Vaginal Lactobacillus fatty acid response mechanisms reveal a metabolite-targeted strategy for bacterial vaginosis treatment. Cell 187, 5413–5430.e5429 (2024).
Google Scholar
Moreno, I. & Franasiak, J. M. Endometrial microbiota-new player in town. Fertil. Steril. 108, 32–39 (2017).
Google Scholar
Baker, J. M., Chase, D. M. & Herbst-Kralovetz, M. M. Uterine microbiota: residents, tourists, or invaders?. Front. Immunol. 9, 208 (2018).
Google Scholar
Tao, X. et al. Characterizing the endometrial microbiome by analyzing the ultra-low bacteria from embryo transfer catheter tips in IVF cycles: next generation sequencing (NGS) analysis of the 16S ribosomal gene. Hum. Microbiome J. 3, 15–21 (2017).
Google Scholar
Mitchell, C. M. et al. Colonization of the upper genital tract by vaginal bacterial species in nonpregnant women. Am. J. Obstet. Gynecol. 212, 611. e611–611. e619 (2015).
Google Scholar
Goodrich, J. K. et al. Human genetics shape the gut microbiome. Cell 159, 789–799 (2014).
Google Scholar
Gao, H. et al. Deciphering the role of female reproductive tract microbiome in reproductive health: a review. Front. Cell Infect. Microbiol. 14, 1351540 (2024).
Google Scholar
Al-Nasiry, S. et al. The interplay between reproductive tract microbiota and immunological system in human reproduction. Front. Immunol. 11, 378 (2020).
Google Scholar
Garcia-Grau, I., Simon, C. & Moreno, I. Uterine microbiome—low biomass and high expectations. Biol. Reprod. 101, 1102–1114 (2018).
Google Scholar
Molina, N. M. et al. New opportunities for endometrial health by modifying uterine microbial composition: present or future? Biomolecules 10, (2020).
Glassing, A., Dowd, S. E., Galandiuk, S., Davis, B. & Chiodini, R. J. Inherent bacterial DNA contamination of extraction and sequencing reagents may affect interpretation of microbiota in low bacterial biomass samples. Gut Pathog. 8, 24 (2016).
Google Scholar
Kim, D. et al. Optimizing methods and dodging pitfalls in microbiome research. Microbiome 5, 52 (2017).
Google Scholar
Semertzidou, A. et al. Microbial signatures and continuum in endometrial cancer and benign patients. Microbiome 12, 118 (2024).
Google Scholar
Liu, Y. et al. Systematic comparison of bacterial colonization of endometrial tissue and fluid samples in recurrent miscarriage patients: implications for future endometrial microbiome studies. Clin. Chem. 64, 1743–1752 (2018).
Google Scholar
Polifke, A. et al. Differential characteristics of vaginal versus endometrial microbiota in IVF patients. Sci. Rep. 14, 30508 (2024).
Google Scholar
Li, F. et al. The metagenome of the female upper reproductive tract. Gigascience 7, (2018).
Blazheva, S. et al. Unlocking the uterine code: microbiota, immune cells, and therapy for recurrent reproductive failure. Microorganisms 12, (2024).
Zhang, R., Wang, M., Zhong, J. & Xue, H. Altered endometrial microbiota profile is associated with poor endometrial receptivity of repeated implantation failure. Am. J. Reprod. Immunol. 92, e70005 (2024).
Google Scholar
Su, W. et al. Vaginal and endometrial microbiome dysbiosis associated with adverse embryo transfer outcomes. Reprod. Biol. Endocrinol. 22, 111 (2024).
Google Scholar
Masucci, L. et al. Celiac disease predisposition and genital tract microbiota in women affected by recurrent pregnancy loss. Nutrients 15, (2023).
Moreno, I. et al. Endometrial microbiota composition is associated with reproductive outcome in infertile patients. Microbiome 10, 1 (2022).
Google Scholar
Peuranpää, P. et al. Female reproductive tract microbiota and recurrent pregnancy loss: a nested case-control study. Reprod. Biomed. Online 45, 1021–1031 (2022).
Google Scholar
Shi, Y., Yamada, H., Sasagawa, Y., Tanimura, K. & Deguchi, M. Uterine endometrium microbiota and pregnancy outcome in women with recurrent pregnancy loss. J. Reprod. Immunol. 152, 103653 (2022).
Google Scholar
Odendaal, J. et al. The endometrial microbiota and early pregnancy loss. Hum. Reprod. 39, 638–646 (2024).
Google Scholar
Hood, R. B. et al. Serum and follicular fluid metabolome and markers of ovarian stimulation. Hum. Reprod. 38, 2196–2207 (2023).
Google Scholar
Molina, N. M. et al. Endometrial whole metabolome profile at the receptive phase: influence of Mediterranean Diet and infertility. Front. Endocrinol. 14, 1120988 (2023).
Google Scholar
Li, K. et al. Association of fatty acids and lipids metabolism in placenta with early spontaneous pregnancy loss in Chinese women. Food Funct. 9, 1179–1186 (2018).
Google Scholar
Wang, L. L. et al. The metabolic landscape of decidua in recurrent pregnancy loss using a global metabolomics approach. Placenta 112, 45–53 (2021).
Google Scholar
Punzón-Jiménez, P. & Labarta, E. The impact of the female genital tract microbiome in women health and reproduction: a review. J. Assist Reprod. Genet 38, 2519–2541 (2021).
Google Scholar
Pelzer, E. S. et al. The fallopian tube microbiome: implications for reproductive health. Oncotarget 9, 21541–21551 (2018).
Google Scholar
Teh, H. E., Pung, C. K., Arasoo, V. J. T. & Yap, P. S. X. A landscape view of the female genital tract microbiome in healthy controls and women with reproductive health conditions associated with ectopic pregnancy. Br. J. Biomed. Sci. 80, 2023 (2024).
Google Scholar
Paradowska, E., Jabłońska, A., Studzińska, M., Wilczyński, M. & Wilczyński, J. R. Detection and genotyping of CMV and HPV in tumors and fallopian tubes from epithelial ovarian cancer patients. Sci. Rep. 9, 19935 (2019).
Google Scholar
Zhou, B. et al. The biodiversity composition of microbiome in ovarian carcinoma patients. Sci. Rep. 9, 1691 (2019).
Google Scholar
Łaniewski, P., Ilhan, Z. E. & Herbst-Kralovetz, M. M. The microbiome and gynaecological cancer development, prevention and therapy. Nat. Rev. Urol. 17, 232–250 (2020).
Google Scholar
Banerjee, S. et al. The ovarian cancer oncobiome. Oncotarget 8, 36225 (2017).
Google Scholar
Sola-Leyva, A. et al. Assessing the ovarian microbiome: lack of a distinguishable microbial signature beyond contamination. Reprod. Biomed. Online 51, 104988 (2025).
Google Scholar
Gosmann, C. et al. Lactobacillus-deficient cervicovaginal bacterial communities are associated with increased HIV acquisition in young South African women. Immunity 46, 29–37 (2017).
Google Scholar
Shannon, B. et al. Distinct effects of the cervicovaginal microbiota and herpes simplex type 2 infection on female genital tract immunology. J. Infect. Dis. 215, 1366–1375 (2017).
Google Scholar
Günther, V. et al. Vaginal microbiome in reproductive medicine. Diagnostics 12, (2022).
Chen, X., Lu, Y., Chen, T. & Li, R. The female vaginal microbiome in health and bacterial vaginosis. Front. Cell. Infect. Microbiol. 11, 631972 (2021).
Google Scholar
Cheng, L. et al. Vaginal microbiota and human papillomavirus infection among young Swedish women. NPJ Biofilms Microbiomes 6, 39 (2020).
Google Scholar
Haggerty, C. L. et al. Identification of novel microbes associated with pelvic inflammatory disease and infertility. Sex. Transm. Infect. 92, 441–446 (2016).
Google Scholar
Ness, R. B. et al. Bacterial vaginosis and risk of pelvic inflammatory disease. Obstet. Gynecol. 104, 761–769 (2004).
Google Scholar
Wang, J. et al. Translocation of vaginal microbiota is involved in impairment and protection of uterine health. Nat. Commun. 12, 4191 (2021).
Google Scholar
Ravel, J., Moreno, I. & Simón, C. Bacterial vaginosis and its association with infertility, endometritis, and pelvic inflammatory disease. Am. J. Obstet. Gynecol. 224, 251–257 (2021).
Google Scholar
Musa, J. et al. Vaginal microbiome community state types and high-risk human papillomaviruses in cervical precancer and cancer in North-central Nigeria. BMC Cancer 23, 683 (2023).
Google Scholar
Kunaseth, J. et al. Vaginal microbiome of women with adenomyosis: a case-control study. PLoS ONE 17, e0263283 (2022).
Google Scholar
Lozano, F. M. et al. Characterization of the vaginal and endometrial microbiome in patients with chronic endometritis. Eur. J. Obstet. Gynecol. Reprod. Biol. 263, 25–32 (2021).
Google Scholar
Han, Y. L. et al. Vaginal microbiome dysbiosis as a novel noninvasive biomarker for detection of chronic endometritis in infertile women. Int. J. Gynecol. Obstet. 167, 1034–1042 (2024).
Google Scholar
Hinderfeld Annabel, S., Phukan, N., Bär, A.-K., Roberton Anthony, M. & Simoes-Barbosa, A. Cooperative Interactions between Trichomonas vaginalis and associated bacteria enhance paracellular permeability of the cervicovaginal epithelium by dysregulating tight junctions. Infect. Immun. 87, e00141–19, (2019).
Google Scholar
To, M. S. et al. Cervical cerclage for prevention of preterm delivery in women with short cervix: randomised controlled trial. Lancet 363, 1849–1853 (2004).
Google Scholar
Wang, K., Wang, K., Wang, J., Yu, F. & Ye, C. Protective effect of Clostridium butyricum on Escherichia coli-induced endometritis in mice via ameliorating endometrial barrier and inhibiting inflammatory response. Microbiol. Spectr. 10, e03286–03222 (2022).
Google Scholar
van Teijlingen, N. H. et al. Vaginal dysbiosis associated-bacteria Megasphaera elsdenii and Prevotella timonensis induce immune activation via dendritic cells. J. Reprod. Immunol. 138, 103085 (2020).
Google Scholar
Zervomanolakis, I. et al. Physiology of upward transport in the human female genital tract. Ann. N. Y. Acad. Sci. 1101, 1–20 (2007).
Google Scholar
Brunham, R. C., Gottlieb, S. L. & Paavonen, J. Pelvic inflammatory disease. N. Engl. J. Med. 372, 2039–2048 (2015).
Google Scholar
Darville, T. Pelvic inflammatory disease due to Neisseria gonorrhoeae and Chlamydia trachomatis: immune evasion mechanisms and pathogenic disease pathways. J. Infect. Dis. 224, S39–s46 (2021).
Google Scholar
Li, X. et al. Biochemical indicators and vaginal microecological abnormalities indicate the occurrence of intrauterine adhesions. Med. Microecol. 11, 100050 (2022).
Google Scholar
Ness, R. B. et al. A cluster analysis of bacterial vaginosis-associated microflora and pelvic inflammatory disease. Am. J. Epidemiol. 162, 585–590 (2005).
Google Scholar
Wiesenfeld, H. C., Hillier, S. L., Krohn, M. A., Landers, D. V. & Sweet, R. L. Bacterial vaginosis is a strong predictor of Neisseria gonorrhoeae and Chlamydia trachomatis infection. Clin. Infect. Dis. 36, 663–668 (2003).
Google Scholar
Sessa, R. et al. Characterization of the vaginal microbiota in Italian women with endometriosis: preliminary study. Arch. Gynecol. Obstet. 310, 2141–2151 (2024).
Google Scholar
Fettweis, J. M. et al. Differences in vaginal microbiome in African American women versus women of European ancestry. Microbiology 160, 2272–2282 (2014).
Google Scholar
Wright, M. L. et al. Vaginal microbiome Lactobacillus crispatus is heritable among European American women. Commun. Biol. 4, 872 (2021).
Google Scholar
Onywera, H., Williamson, A. L., Mbulawa, Z. Z. A., Coetzee, D. & Meiring, T. L. Factors associated with the composition and diversity of the cervical microbiota of reproductive-age Black South African women: a retrospective cross-sectional study. PeerJ 7, e7488 (2019).
Google Scholar
Yang, Q. et al. Translocation of vaginal and cervical low-abundance non-Lactobacillus bacteria notably associate with endometriosis: a pilot study. Micro. Pathog. 183, 106309 (2023).
Google Scholar
Peng, N., Xiao, J., He, L. & Xie, L. Association between vaginal microecological alterations and high-risk human papillomavirus infection: a cross-sectional study. Front. Cell Infect. Microbiol. 15, 1618846 (2025).
Google Scholar
Mabaso, N. G. et al. The vaginal microbiome of South African pregnant women living with human immunodeficiency virus (HIV) with and without Chlamydia trachomatis infection. BMC Women’s Health 24, 410 (2024).
Google Scholar
de Angelis, C. et al. Smoke, alcohol and drug addiction and female fertility. Reprod. Biol. Endocrinol. 18, 21 (2020).
Google Scholar
Skakkebæk, N. E. et al. Environmental factors in declining human fertility. Nat. Rev. Endocrinol. 18, 139–157 (2022).
Google Scholar
Gudnadottir, U. et al. Pre-pregnancy complications – associated factors and wellbeing in early pregnancy: a Swedish cohort study. BMC Pregnancy Childbirth 23, 153 (2023).
Google Scholar
Darıcı, E. et al. From body mass index to body composition in female infertility. Reprod. Biomed. Online 51, 104941 (2025).
Google Scholar
Sun, M., Lu, Y., Yang, X. & Mao, X. Association between relative fat mass and sterility in women of reproductive age in the United States: results from the 2013-2018 NHANES. Front. Endocrinol. 16, 1521247 (2025).
Google Scholar
Eslami, M. et al. Microbiome structure in healthy and pregnant women and importance of vaginal dysbiosis in spontaneous abortion. Front. Cell Infect. Microbiol. 14, 1401610 (2024).
Google Scholar
Cattelan, S., Devigili, A., Santacà, M. & Gasparini, C. Female reproductive fluid attracts more and better sperm: implications for within-ejaculate cryptic female choice. Biol. Lett. 19, 20230063 (2023).
Google Scholar
Moore, D. E. et al. Bacteria in the transfer catheter tip influence the live-birth rate after in vitro fertilization. Fertil. Steril. 74, 1118–1124 (2000).
Google Scholar
Bayar, E., Bennett, P. R., Chan, D., Sykes, L. & MacIntyre, D. A. The pregnancy microbiome and preterm birth. Semin. Immunopathol. 42, 487–499 (2020).
Google Scholar
Xiao, L., Zhou, T., Zuo, Z., Sun, N. & Zhao, F. Spatiotemporal patterns of the pregnancy microbiome and links to reproductive disorders. Sci. Bull. 69, 1275–1285 (2024).
Google Scholar
Zhou, T., Xiao, L., Zuo, Z. & Zhao, F. MAMI: a comprehensive database of mother–infant microbiome and probiotic resources. Nucleic Acids Res. 52, D738–D746 (2023).
Google Scholar
Wang, T. et al. Vaginal microbiota are associated with in vitro fertilization during female infertility. iMeta 3, e185 (2024).
Google Scholar
Severgnini, M. et al. A deep look at the vaginal environment during pregnancy and puerperium. Front. Cell. Infect. Microbiol. 12, (2022).
Marangoni, A. et al. New insights into vaginal environment during pregnancy. Front. Mol. Biosci. 8, 656844 (2021).
Google Scholar
Mastromarino, P. et al. Biological control of vaginosis to improve reproductive health. Indian J. Med. Res. 140, S91–S97 (2014).
Google Scholar
Gudnadottir, U. et al. The vaginal microbiome and the risk of preterm birth: a systematic review and network meta-analysis. Sci. Rep. 12, 7926 (2022).
Google Scholar
Liu, F.-T. et al. An Altered Microbiota In The Lower And Upper Female Reproductive Tract Of Women With Recurrent Spontaneous Abortion. Microbiol. Spectr. 10, e00462–00422 (2022).
Google Scholar
Al-Memar, M. et al. The association between vaginal bacterial composition and miscarriage: a nested case–control study. BJOG 127, 264–274 (2020).
Google Scholar
Xu, L. et al. Vaginal microbiota diversity of patients with embryonic miscarriage by using 16S rDNA high-throughput sequencing. Int. J. Genomics 2020, 1764959 (2020).
Google Scholar
Fan, T. et al. The alteration and potential relationship of vaginal microbiota and chemokines for unexplained recurrent spontaneous abortion. Medecine 99, e23558 (2020).
Google Scholar
Campisciano, G. et al. Subclinical alteration of the cervical-vaginal microbiome in women with idiopathic infertility. J. Cell. Physiol. 232, 1681–1688 (2017).
Google Scholar
Campisciano, G. et al. Lactobacillus iners and gasseri, Prevotella bivia and HPV belong to the microbiological signature negatively affecting human reproduction. Microorganisms 9, (2020).
Bernabeu, A. et al. Effect of the vaginal microbiome on the pregnancy rate in women receiving assisted reproductive treatment. J. Assist. Reprod. Genet. 36, 2111–2119 (2019).
Google Scholar
Koedooder, R. et al. The vaginal microbiome as a predictor for outcome of in vitro fertilization with or without intracytoplasmic sperm injection: a prospective study. Hum. Reprod. 34, 1042–1054 (2019).
Google Scholar
Jiao, X. et al. Alteration of vaginal microbiota in patients with recurrent miscarriage. J. Obstet. Gynaecol. 42, 248–255 (2022).
Google Scholar
McDonald, H. M. & Chambers, H. M. Intrauterine infection and spontaneous midgestation abortion: is the spectrum of microorganisms similar to that in preterm labor?. Infect. Dis. Obstet. Gynecol. 8, 220–227 (2000).
Google Scholar
Laghi, L. et al. Vaginal metabolic profiles during pregnancy: changes between first and second trimester. PLoS ONE 16, e0249925 (2021).
Google Scholar
Kindschuh, W. F. et al. Preterm birth is associated with xenobiotics and predicted by the vaginal metabolome. Nat. Microbiol 8, 246–259 (2023).
Google Scholar
Liu, L. et al. Detection of vaginal metabolite changes in premature rupture of membrane patients in third trimester pregnancy: a prospective cohort study. Reprod. Sci. 28, 585–594 (2021).
Google Scholar
Goldstein, S. R., Siddhanti, S., Ciaccia, A. V. & Plouffe, L. Jr. A pharmacological review of selective oestrogen receptor modulators. Hum. Reprod. Update 6, 212–224 (2000).
Google Scholar
Berridge, M. J. The inositol trisphosphate/calcium signaling pathway in health and disease. Physiol. Rev. 96, 1261–1296 (2016).
Google Scholar
Cerdeira, A. S. et al. Conversion of peripheral blood NK cells to a decidual NK-like phenotype by a cocktail of defined factors. J. Immunol. 190, 3939–3948 (2013).
Google Scholar
Benner, M., Ferwerda, G., Joosten, I. & van der Molen, R. G. How uterine microbiota might be responsible for a receptive, fertile endometrium. Hum. Reprod. Update 24, 393–415 (2018).
Google Scholar
Omenetti, S. & Pizarro, T. T. The treg/Th17 axis: a dynamic balance regulated by the gut microbiome. Front. Immunol. 6, 639 (2015).
Google Scholar
Gaboriau-Routhiau, V. et al. The key role of segmented filamentous bacteria in the coordinated maturation of gut helper T cell responses. Immunity 31, 677–689 (2009).
Google Scholar
Iijima, N., Mattei, L. M. & Iwasaki, A. Recruited inflammatory monocytes stimulate antiviral Th1 immunity in infected tissue. Proc. Natl. Acad. Sci. USA 108, 284–289 (2011).
Google Scholar
Rodriguez, A. et al. Requirement of bic/microRNA-155 for normal immune function. Science 316, 608–611 (2007).
Google Scholar
Nagy, Z., Herbison, A., Kwakowsky, A., Kovacs, G. & Barabas, K. Editorial: Estrogen effects on fertility and neurodegeneration-classical versus non-classical actions. Front. Endocrinol. 14, 1192671 (2023).
Google Scholar
Qi, X. et al. Gut microbiota-bile acid-interleukin-22 axis orchestrates polycystic ovary syndrome. Nat. Med. 25, 1225–1233 (2019).
Google Scholar
Joshi, A. PCOS stratification for precision diagnostics and treatment. Front. Cell. Dev. Biol. 12, 1358755 (2024).
Google Scholar
Chon, S. J., Umair, Z. & Yoon, M. S. Premature ovarian insufficiency: past, present, and future. Front. Cell. Dev. Biol. 9, 672890 (2021).
Google Scholar
Plottel, C. laudiaS. & Blaser, M. artinJ. Microbiome and malignancy. Cell Host Microbe 10, 324–335 (2011).
Google Scholar
Kwa, M., Plottel, C. S., Blaser, M. J. & Adams, S. The intestinal microbiome and estrogen receptor-positive female breast cancer. J. Natl. Cancer Inst. 108, (2016).
Baker, J. M., Al-Nakkash, L. & Herbst-Kralovetz, M. M. Estrogen-gut microbiome axis: physiological and clinical implications. Maturitas 103, 45–53 (2017).
Google Scholar
Hu, S. et al. Gut microbial beta-glucuronidase: a vital regulator in female estrogen metabolism. Gut Microbes 15, 2236749 (2023).
Google Scholar
Lombard, V., Golaconda Ramulu, H., Drula, E., Coutinho, P. M. & Henrissat, B. The carbohydrate-active enzymes database (CAZy) in 2013. Nucleic Acids Res 42, D490–D495 (2014).
Google Scholar
An, J., Kwon, H., Lim, W. & Moon, B. I. Staphylococcus aureus-derived extracellular vesicles enhance the efficacy of endocrine therapy in breast cancer cells. J. Clin. Med. 11, (2022).
Salliss, M. E., Farland, L. V., Mahnert, N. D. & Herbst-Kralovetz, M. M. The role of gut and genital microbiota and the estrobolome in endometriosis, infertility and chronic pelvic pain. Hum. Reprod. Update 28, 92–131 (2021).
Google Scholar
Chambers, L. M. et al. Disruption of the gut microbiota confers cisplatin resistance in epithelial ovarian cancer. Cancer Res. 82, 4654–4669 (2022).
Google Scholar
Laschke, M. W. & Menger, M. D. The gut microbiota: a puppet master in the pathogenesis of endometriosis?. Am. J. Obstet. Gynecol. 215, 68.e61–64 (2016).
Google Scholar
Pollet, R. M. et al. An atlas of β-glucuronidases in the human intestinal microbiome. Structure 25, 967–977.e965 (2017).
Google Scholar
Williams, C. L., Garcia-Reyero, N., Martyniuk, C. J., Tubbs, C. W. & Bisesi, J. H. Jr. Regulation of endocrine systems by the microbiome: perspectives from comparative animal models. Gen. Comp. Endocrinol. 292, 113437 (2020).
Google Scholar
Wang, X. et al. Microbiota dysbiosis in primary Sjögren’s syndrome and the ameliorative effect of hydroxychloroquine. Cell Rep. 40, (2022).
Patel, S. Polycystic ovary syndrome (PCOS), an inflammatory, systemic, lifestyle endocrinopathy. J. Steroid Biochem. Mol. Biol. 182, 27–36 (2018).
Google Scholar
Thackray, V. G. Sex, microbes, and polycystic ovary syndrome. Trends Endocrinol. Metab. 30, 54–65 (2019).
Google Scholar
Liu, R. et al. Dysbiosis of gut microbiota associated with clinical parameters in polycystic ovary syndrome. Front. Microbiol. 8, 324 (2017).
Google Scholar
Jobira, B. et al. Obese adolescents with PCOS have altered biodiversity and relative abundance in gastrointestinal microbiota. J. Clin. Endocrinol. Metab. 105, e2134–e2144 (2020).
Google Scholar
Chu, W. et al. Metagenomic analysis identified microbiome alterations and pathological association between intestinal microbiota and polycystic ovary syndrome. Fertil. Steril. 113, 1286–1298. e1284 (2020).
Google Scholar
Wu, J. et al. Association between premature ovarian insufficiency and gut microbiota. BMC Pregnancy Childbirth 21, 418 (2021).
Google Scholar
Elkafas, H., Walls, M., Al-Hendy, A. & Ismail, N. Gut and genital tract microbiomes: dysbiosis and link to gynecological disorders. Front. Cell. Infect. Microbiol. 12, (2022).
Hu, L., Zhang, J., Lu, Y., Fu, B. & Hu, W. Estrogen receptor beta promotes endometriosis progression by upregulating CD47 expression in ectopic endometrial stromal cells. J. Reprod. Immunol. 151, 103513 (2022).
Google Scholar
Dyson, M. T. & Bulun, S. E. Cutting SRC-1 down to size in endometriosis. Nat. Med. 18, 1016–1018 (2012).
Google Scholar
Scarfò, G. et al. Endometrial dysbiosis: a possible association with estrobolome alteration. Biomolecules 14, (2024).
Mikhael, S., Punjala-Patel, A. & Gavrilova-Jordan, L. Hypothalamic-pituitary-ovarian axis disorders impacting female fertility. Biomedicines 7, (2019).
Qi, Q. et al. Update on the pathogenesis of endometriosis-related infertility based on contemporary evidence. Front. Endocrinol. 16, 1558271 (2025).
Google Scholar
Zhao, X., Shi, W., Li, Z. & Zhang, W. Linking reproductive tract microbiota to premature ovarian insufficiency: pathophysiological mechanisms and therapies. J. Reprod. Immunol. 166, 104325 (2024).
Google Scholar
Wu, J. et al. Characteristics of the vaginal microbiome in women with premature ovarian insufficiency. J. Ovarian Res 14, 172 (2021).
Google Scholar
Tremellen, K. & Pearce, K. Dysbiosis of gut microbiota (DOGMA)-a novel theory for the development of polycystic ovarian syndrome. Med. Hypotheses 79, 104–112 (2012).
Google Scholar
Lagathu, C. et al. Chronic interleukin-6 (IL-6) treatment increased IL-6 secretion and induced insulin resistance in adipocyte: prevention by rosiglitazone. Biochem. Biophys. Res. Commun. 311, 372–379 (2003).
Google Scholar
Hotamisligil, G. S. et al. IRS-1-mediated inhibition of insulin receptor tyrosine kinase activity in TNF-α- and obesity-induced insulin resistance. Science 271, 665–668 (1996).
Google Scholar
Senthilkumar, H. & Arumugam, M. Gut microbiota: a hidden player in polycystic ovary syndrome. J. Transl. Med 23, 443 (2025).
Google Scholar
Bashir, Z. et al. Investigations of microbiota composition and neuroactive pathways in association with symptoms of stress and depression in a cohort of healthy women. Front. Cell Infect. Microbiol. 14, 1324794 (2024).
Google Scholar
Das, S., Bhattacharjee, M. J., Mukherjee, A. K. & Khan, M. R. Recent advances in understanding of multifaceted changes in the vaginal microenvironment: implications in vaginal health and therapeutics. Crit. Rev. Microbiol. 49, 256–282 (2023).
Google Scholar
Velraeds, M. M., van der Mei, H. C., Reid, G. & Busscher, H. J. Inhibition of initial adhesion of uropathogenic Enterococcus faecalis by biosurfactants from Lactobacillus isolates. Appl. Environ. Microbiol. 62, 1958–1963 (1996).
Google Scholar
Takano, T. et al. Inhibitory effects of vaginal Lactobacilli on Candida albicans growth, hyphal formation, biofilm development, and epithelial cell adhesion. Front. Cell Infect. Microbiol 13, 1113401 (2023).
Google Scholar
Melian, C., Segli, F., Gonzalez, R., Vignolo, G. & Castellano, P. Lactocin AL705 as quorum sensing inhibitor to control Listeria monocytogenes biofilm formation. J. Appl. Microbiol. 127, 911–920 (2019).
Google Scholar
Gudiña, E. J., Teixeira, J. A. & Rodrigues, L. R. Isolation and functional characterization of a biosurfactant produced by Lactobacillus paracasei. Colloid Surf. B-Biointerfaces 76, 298–304 (2010).
Google Scholar
De Gregorio, P. R. et al. Biosurfactant from vaginal Lactobacillus crispatus BC1 as a promising agent to interfere with Candida adhesion. Microb. Cell. Fact. 19, 133 (2020).
Google Scholar
Nunn, K. L. et al. Enhanced trapping of HIV-1 by human cervicovaginal mucus is associated with Lactobacillus crispatus-dominant microbiota. mBio 6, e01084–01015 (2015).
Google Scholar
Hoang, T. et al. The cervicovaginal mucus barrier to HIV-1 is diminished in bacterial vaginosis. PLoS Pathog. 16, e1008236 (2020).
Google Scholar
Castro, J., Martins, A. P., Rodrigues, M. E. & Cerca, N. Lactobacillus crispatus represses vaginolysin expression by BV associated Gardnerella vaginalis and reduces cell cytotoxicity. Anaerobe 50, 60–63 (2018).
Google Scholar
Zhao, W., Wang, J., Li, X., Li, Y. & Ye, C. Deoxycholic acid inhibits Staphylococcus aureus-induced endometritis through regulating TGR5/PKA/NF-κB signaling pathway. Int. Immunopharmacol. 118, 110004 (2023).
Google Scholar
Hedges, S. R., Barrientes, F., Desmond, R. A. & Schwebke, J. R. Local and systemic cytokine levels in relation to changes in vaginal flora. J. Infect. Dis. 193, 556–562 (2006).
Google Scholar
Beigi, R. H., Yudin, M. H., Cosentino, L., Meyn, L. A. & Hillier, S. L. Cytokines, pregnancy, and bacterial vaginosis: comparison of levels of cervical cytokines in pregnant and nonpregnant women with bacterial vaginosis. J. Infect. Dis. 196, 1355–1360 (2007).
Google Scholar
Joo, H. M. et al. Lactobacillus johnsonii HY7042 ameliorates Gardnerella vaginalis-induced vaginosis by killing Gardnerella vaginalis and inhibiting NF-κB activation. Int. Immunopharmacol. 11, 1758–1765 (2011).
Google Scholar
Decout, A. et al. Lactobacillus crispatus S-layer proteins modulate innate immune response and inflammation in the lower female reproductive tract. Nat. Commun. 15, 10879 (2024).
Google Scholar
Glick, V. J. et al. Vaginal lactobacilli produce anti-inflammatory β-carboline compounds. Cell Host Microbe 32, 1897–1909.e1897 (2024).
Google Scholar
Hemmerling, A. et al. Effect of the vaginal live biotherapeutic LACTIN-V (Lactobacillus crispatus CTV-05) on vaginal microbiota and genital tract inflammation among women at high risk of HIV acquisition in South Africa: a phase 2, randomised, placebo-controlled trial. Lancet Microbe 6, 101037 (2025).
Google Scholar
Li, C. et al. Alleviative effect of vaginal lactobacilli with probiotic potential from healthy Chinese women on bacterial vaginosis caused by Gardnerella vaginalis in mice. Probiotics Antimicrob Proteins (2025).
Iwami, N. et al. Therapeutic intervention based on gene sequencing analysis of microbial 16S ribosomal RNA of the intrauterine microbiome improves pregnancy outcomes in IVF patients: a prospective cohort study. J. Assist. Reprod. Genet. 40, 125–135 (2023).
Google Scholar
He, X. et al. The therapeutic potential of Lactobacillus crispatus for chronic endometritis: a comprehensive clinical trial and experimental investigation. Probiotics Antimicrob. Proteins (2024).
Fan, G. et al. Lactobacillus-loaded easily injectable hydrogel promotes endometrial repair via long-term retention and microenvironment modulation. ACS Nano (2025).
Wang, W. J. et al. Endometrial TGF-β, IL-10, IL-17 and autophagy are dysregulated in women with recurrent implantation failure with chronic endometritis. Reprod. Biol. Endocrinol. 17, 2 (2019).
Google Scholar
Tian, Y. et al. Follicular helper T lymphocytes in the endometria of patients with reproductive failure: association with pregnancy outcomes and inflammatory status of the endometria. Am. J. Reprod. Immunol. 90, e13708 (2023).
Google Scholar
Kitazawa, J. et al. Alteration in endometrial helper T-cell subgroups in chronic endometritis. Am. J. Reprod. Immunol. 85, e13372 (2021).
Google Scholar
Chen, P., Chen, P., Guo, Y., Fang, C. & Li, T. Interaction between chronic endometritis caused endometrial microbiota disorder and endometrial immune environment change in recurrent implantation failure. Front. Immunol. 12, 748447 (2021).
Google Scholar
Chaouat, G. The Th1/Th2 paradigm: still important in pregnancy?. Semin. Immunopathol. 29, 95–113 (2007).
Google Scholar
Guo, M. et al. Lactobacillus rhamnosus GG ameliorates osteoporosis in ovariectomized rats by regulating the Th17/Treg balance and gut microbiota structure. Gut Microbes 15, 2190304 (2023).
Google Scholar
Fan, L. et al. B. adolescentis ameliorates chronic colitis by regulating Treg/Th2 response and gut microbiota remodeling. Gut Microbes 13, 1–17 (2021).
Google Scholar
Dwivedi, M., Kumar, P., Laddha, N. C. & Kemp, E. H. Induction of regulatory T cells: a role for probiotics and prebiotics to suppress autoimmunity. Autoimmun. Rev. 15, 379–392 (2016).
Google Scholar
Cocomazzi, G. et al. Refining unfavorable vaginal microbial community in infertile women subjected to precision probiotic intervention: an exploratory single-arm, prospective, open-label, interventional study. Microorganisms 13, (2025).
Chen, X., Sui, Y., Gu, J., Wang, L. & Sun, N. The implication of the vaginal microbiome in female infertility and assisted conception outcomes. Genomics Proteomics Bioinform. (2025).
Sengupta, M. et al. Biofilm producing enterococcus isolates from vaginal microbiota. Antibiotics 10, (2021).
Freitas, A. C. & Hill, J. E. Quantification, isolation and characterization of Bifidobacterium from the vaginal microbiomes of reproductive aged women. Anaerobe 47, 145–156 (2017).
Google Scholar
Shin, Y. J., Ma, X., Joo, M. K., Baek, J. S. & Kim, D. H. Lactococcus lactis and Bifidobacterium bifidum alleviate postmenopausal symptoms by suppressing NF-κB signaling and microbiota dysbiosis. Sci. Rep. 14, 31675 (2024).
Google Scholar
Kim, D. E. et al. Lactobacillus plantarum NK3 and Bifidobacterium longum NK49 alleviate bacterial vaginosis and osteoporosis in mice by suppressing NF-κB-linked TNF-α expression. J. Med. Food 22, 1022–1031 (2019).
Google Scholar
Nori, S. R. C. et al. Strain-level variation among vaginal Lactobacillus crispatus and Lactobacillus iners as identified by comparative metagenomics. NPJ Biofilms Microbiomes 11, 49 (2025).
Google Scholar
Sanders, M. E. et al. Safety assessment of probiotics for human use. Gut Microbes 1, 164–185 (2010).
Google Scholar
Li, S. et al. Alleviation of Limosilactobacillus reuteri in polycystic ovary syndrome protects against circadian dysrhythmia-induced dyslipidemia via capric acid and GALR1 signaling. npj Biofilms Microbomes 9, (2023).
Canfora, E. E., Jocken, J. W. & Blaak, E. E. Short-chain fatty acids in control of body weight and insulin sensitivity. Nat. Rev. Endocrinol. 11, 577–591 (2015).
Google Scholar
Singh, V., Mahra, K., Jung, D. & Shin, J. H. Gut microbes in polycystic ovary syndrome and associated comorbidities; type 2 diabetes, non-alcoholic fatty liver disease (NAFLD), cardiovascular disease (CVD), and the potential of microbial therapeutics. Probiotics Antimicrob. Proteins (2024).
He, Y. et al. Lactic acid bacteria alleviate polycystic ovarian syndrome by regulating sex hormone related gut microbiota. Food Funct. 11, 5192–5204 (2020).
Google Scholar
El Hayek, S., Bitar, L., Hamdar, L. H., Mirza, F. G. & Daoud, G. Poly cystic ovarian syndrome: an updated overview. Front. Physiol. 7, 124 (2016).
Google Scholar
Zhang, J. et al. Probiotic Bifidobacterium lactis V9 regulates the secretion of sex hormones in polycystic ovary syndrome patients through the gut-brain axis. mSystems 4, (2019).
Canfora, E. E., Meex, R. C. R., Venema, K. & Blaak, E. E. Gut microbial metabolites in obesity, NAFLD and T2DM. Nat. Rev. Endocrinol. 15, 261–273 (2019).
Google Scholar
Torres, P. J. et al. Gut microbial diversity in women with polycystic ovary syndrome correlates with hyperandrogenism. J. Clin. Endocrinol. Metab. 103, 1502–1511 (2018).
Google Scholar
Rajilić-Stojanović, M. & de Vos, W. M. The first 1000 cultured species of the human gastrointestinal microbiota. Fems Microbiol. Rev. 38, 996–1047 (2014).
Google Scholar
O’Callaghan, A. & van Sinderen, D. Bifidobacteria and their role as members of the human gut microbiota. Front. Microbiol. 7, 925 (2016).
Google Scholar
Chadchan, S. B. et al. Gut microbiota-derived short-chain fatty acids protect against the progression of endometriosis. Life Sci. Alliance 4, (2021).
Kim, N. & Yang, C. Butyrate as a potential modulator in gynecological disease progression. Nutrients 16, (2024).
Zeng, Y., Wu, Y., Zhang, Q. & Xiao, X. Crosstalk between glucagon-like peptide 1 and gut microbiota in metabolic diseases. mBio 15, e0203223 (2024).
Google Scholar
Everard, A. & Cani, P. D. Gut microbiota and GLP-1. Rev. Endocr. Metab. Disord. 15, 189–196 (2014).
Google Scholar
Gallwitz, B. Glucagon-like peptide-1 and gastric inhibitory polypeptide: new advances. Curr. Opin. Endocrinol. Diabetes Obes. 23, 23–27 (2016).
Google Scholar
Oteng, A. B. & Liu, L. GPCR-mediated effects of fatty acids and bile acids on glucose homeostasis. Front. Endocrinol. 14, 1206063 (2023).
Google Scholar
Kimura, I., Ichimura, A., Ohue-Kitano, R. & Igarashi, M. Free fatty acid receptors in health and disease. Physiol. Rev. 100, 171–210 (2020).
Google Scholar
Yadav, H., Lee, J. H., Lloyd, J., Walter, P. & Rane, S. G. Beneficial metabolic effects of a probiotic via butyrate-induced GLP-1 hormone secretion. J. Biol. Chem. 288, 25088–25097 (2013).
Google Scholar
Amabebe, E. & Anumba, D. O. C. Female gut and genital tract microbiota-induced crosstalk and differential effects of short-chain fatty acids on immune sequelae. Front Immunol. 11, 2184 (2020).
Google Scholar
Yao, X. et al. Gut microbiota-derived short chain fatty acids are associated with clinical pregnancy outcome in women undergoing IVF/ICSI-ET: a retrospective study. Nutrients 15, (2023).
Qin, X. et al. Short-chain fatty acids in fetal development and metabolism. Trends Mol. Med. (2024).
Nuriel-Ohayon, M., Neuman, H. & Koren, O. Microbial Changes during Pregnancy, Birth, and Infancy. Front. Microbiol. 7, 1031 (2016).
Google Scholar
Chen, S. et al. Expression and clinical significance of short-chain fatty acids in pregnancy complications. Front. Cell Infect. Microbiol. 12, 1071029 (2022).
Google Scholar
Markowiak-Kopeć, P. & Śliżewska, K. The effect of probiotics on the production of short-chain fatty acids by human intestinal microbiome. Nutrients 12, (2020).
Gao, S. & Wang, J. Maternal and infant microbiome: next-generation indicators and targets for intergenerational health and nutrition care. Protein Cell 14, 807–823 (2023).
Google Scholar
Aron-Wisnewsky, J. et al. Gut microbiota and human NAFLD: disentangling microbial signatures from metabolic disorders. Nat. Rev. Gastroenterol. Hepatol. 17, 279–297 (2020).
Google Scholar
Bustamante, J. M. et al. Impact of fecal microbiota transplantation on gut bacterial bile acid metabolism in humans. Nutrients 14, (2022).
Zhang, C. et al. Lactobacillus reuteri J1 prevents obesity by altering the gut microbiota and regulating bile acid metabolism in obese mice. Food Funct. 13, 6688–6701 (2022).
Google Scholar
Pushpass, R. G., Alzoufairi, S., Jackson, K. G. & Lovegrove, J. A. Circulating bile acids as a link between the gut microbiota and cardiovascular health: impact of prebiotics, probiotics and polyphenol-rich foods. Nutr. Res. Rev. 35, 161–180 (2022).
Google Scholar
Foley, M. H. et al. Lactobacillus bile salt hydrolase substrate specificity governs bacterial fitness and host colonization. Proc. Natl. Acad. Sci. USA. 118, (2021).
Öner, Ö, Aslim, B. & Aydaş, S. B. Mechanisms of cholesterol-lowering effects of lactobacilli and bifidobacteria strains as potential probiotics with their bsh gene analysis. J. Mol. Microbiol. Biotechnol. 24, 12–18 (2014).
Google Scholar
Jones, M. L., Martoni, C. J. & Prakash, S. Cholesterol lowering and inhibition of sterol absorption by Lactobacillus reuteri NCIMB 30242: a randomized controlled trial. Eur. J. Clin. Nutr. 66, 1234–1241 (2012).
Google Scholar
Tang, B. et al. Gut microbiota alters host bile acid metabolism to contribute to intrahepatic cholestasis of pregnancy. Nat. Commun. 14, 1305 (2023).
Google Scholar
Studer, N. et al. Functional intestinal bile acid 7α-dehydroxylation by Clostridium scindens associated with protection from Clostridium difficile infection in a gnotobiotic mouse model. Front. Cell Infect. Microbiol. 6, 191 (2016).
Google Scholar
Kang, J. D. et al. Bile acid 7α-dehydroxylating gut bacteria secrete antibiotics that inhibit Clostridium difficile: role of secondary bile acids. Cell Chem. Biol. 26, 27–34.e24 (2019).
Google Scholar
Song, X. et al. Microbial bile acid metabolites modulate gut RORγ(+) regulatory T cell homeostasis. Nature 577, 410–415 (2020).
Google Scholar
Hang, S. et al. Bile acid metabolites control T(H)17 and T(reg) cell differentiation. Nature 576, 143–148 (2019).
Google Scholar
Figueiredo, A. S. & Schumacher, A. The T helper type 17/regulatory T cell paradigm in pregnancy. Immunology 148, 13–21 (2016).
Google Scholar
Prins, J. R., Gomez-Lopez, N. & Robertson, S. A. Interleukin-6 in pregnancy and gestational disorders. J. Reprod. Immunol. 95, 1–14 (2012).
Google Scholar
Zenclussen, A. C. et al. Murine abortion is associated with enhanced interleukin-6 levels at the feto-maternal interface. Cytokine 24, 150–160 (2003).
Google Scholar
Parsaei, M. et al. The association of serum total bile acid levels with gestational diabetes mellitus: a systematic review and meta-analysis. BMC Pregnancy Childbirth 24, 744 (2024).
Google Scholar
Zhang, J. et al. Elevated maternal serum bile acids level, hypertensive disorders of pregnancy and adverse fetal outcomes: a cohort study of 117,789 pregnant women in China. Clin. Chim. Acta 562, 119896 (2024).
Google Scholar
Zheng, X. et al. Hyocholic acid species improve glucose homeostasis through a distinct TGR5 and FXR signaling mechanism. Cell Metab. 33, 791–803.e797 (2021).
Google Scholar
Rigby, R. J., Knight, S. C., Kamm, M. A. & Stagg, A. J. Production of interleukin (IL)-10 and IL-12 by murine colonic dendritic cells in response to microbial stimuli. Clin. Exp. Immunol. 139, 245–256 (2005).
Google Scholar
Kwon, H. K. et al. Generation of regulatory dendritic cells and CD4+Foxp3+ T cells by probiotics administration suppresses immune disorders. Proc. Natl. Acad. Sci. USA 107, 2159–2164 (2010).
Google Scholar
Hoarau, C., Lagaraine, C., Martin, L., Velge-Roussel, F. & Lebranchu, Y. Supernatant of Bifidobacterium breve induces dendritic cell maturation, activation, and survival through a Toll-like receptor 2 pathway. J. Allergy Clin. Immunol. 117, 696–702 (2006).
Google Scholar
Jiang, L. et al. Hormone replacement therapy reverses gut microbiome and serum metabolome alterations in premature ovarian insufficiency. Front. Endocrinol. 12, 794496 (2021).
Google Scholar
Guo, X. et al. BCAA insufficiency leads to premature ovarian insufficiency via ceramide-induced elevation of ROS. EMBO Mol. Med. 15, e17450 (2023).
Google Scholar
Shi, Y. Q. et al. Premature ovarian insufficiency: a review on the role of oxidative stress and the application of antioxidants. Front. Endocrinol. 14, 1172481 (2023).
Google Scholar
Gojda, J. & Cahova, M. Gut microbiota as the link between elevated BCAA serum levels and insulin resistance. Biomolecules 11, (2021).
Tan, C. et al. The role of gut microbiota and amino metabolism in the effects of improvement of islet β-cell function after modified jejunoileal bypass. Sci. Rep. 11, 4809 (2021).
Google Scholar
Moran-Ramos, S. et al. A higher bacterial inward BCAA transport driven by Faecalibacterium prausnitzii is associated with lower serum levels of BCAA in early adolescents. Mol. Med. 27, 108 (2021).
Google Scholar
Agus, A., Clément, K. & Sokol, H. Gut microbiota-derived metabolites as central regulators in metabolic disorders. Gut 70, 1174–1182 (2021).
Google Scholar
Pedersen, H. K. et al. Human gut microbes impact host serum metabolome and insulin sensitivity. Nature 535, 376–381 (2016).
Google Scholar
Allison, M. J., Baetz, A. L. & Wiegel, J. Alternative pathways for biosynthesis of leucine and other amino acids in Bacteroides ruminicola and Bacteroides fragilis. Appl. Environ. Microbiol. 48, 1111–1117 (1984).
Google Scholar
McCann, J. R. & Rawls, J. F. Essential amino acid metabolites as chemical mediators of host-microbe interaction in the gut. Annu. Rev. Microbiol. 77, 479–497 (2023).
Google Scholar
Wang, H. et al. Gut microbiota metabolism of branched-chain amino acids and their metabolites can improve the physiological function of aging mice. Aging Cell 24, e14434 (2025).
Google Scholar
Rondanelli, M. et al. Effectiveness of a novel food composed of leucine, omega-3 fatty acids and probiotic Lactobacillus paracasei PS23 for the treatment of sarcopenia in elderly subjects: a 2-month randomized double-blind placebo-controlled trial. Nutrients 14, (2022).
Chu, C. et al. Lactobacillus plantarum CCFM405 against rotenone-induced parkinson’s disease mice via regulating gut microbiota and branched-chain amino acids biosynthesis. Nutrients 15, (2023).
Martin, P. M. & Sutherland, A. E. Exogenous amino acids regulate trophectoderm differentiation in the mouse blastocyst through an mTOR-dependent pathway. Dev. Biol. 240, 182–193 (2001).
Google Scholar
Caetano, L. et al. Blastocyst trophectoderm endocytic activation, a marker of adverse developmental programming. Reproduction 162, 289–306 (2021).
Google Scholar
González, I. M. et al. Leucine and arginine regulate trophoblast motility through mTOR-dependent and independent pathways in the preimplantation mouse embryo. Dev. Biol. 361, 286–300 (2012).
Google Scholar
Van Winkle, L. J. Amino acid transport regulation and early embryo development. Biol. Reprod. 64, 1–12 (2001).
Google Scholar
Teodoro, G. F. et al. Leucine is essential for attenuating fetal growth restriction caused by a protein-restricted diet in rats. J. Nutr. 142, 924–930 (2012).
Google Scholar
Mogami, H. et al. Isocaloric high-protein diet as well as branched-chain amino acids supplemented diet partially alleviates adverse consequences of maternal undernutrition on fetal growth. Growth Horm. IGF Res. 19, 478–485 (2009).
Google Scholar
Zhang, S., Zeng, X., Ren, M., Mao, X. & Qiao, S. Novel metabolic and physiological functions of branched chain amino acids: a review. J. Anim. Sci. Biotechnol. 8, 10 (2017).
Google Scholar
Rehnitz, J. et al. Activation of AKT/mammalian target of rapamycin signaling in the peripheral blood of women with premature ovarian insufficiency and its correlation with FMR1 expression. Reprod. Biol. Endocrinol. 20, 44 (2022).
Google Scholar
Zhang, X. et al. Enhanced glycolysis in granulosa cells promotes the activation of primordial follicles through mTOR signaling. Cell Death Dis. 13, 87 (2022).
Google Scholar
Dou, X. et al. Bu-Shen-Ning-Xin decoction alleviates premature ovarian insufficiency (POI) by regulating autophagy of granule cells through activating PI3K/AKT/mTOR pathway. Gynecol. Endocrinol. 38, 754–764 (2022).
Google Scholar
Lu, X. et al. hUMSC transplantation restores ovarian function in POI rats by inhibiting autophagy of theca-interstitial cells via the AMPK/mTOR signaling pathway. Stem Cell Res. Ther. 11, 268 (2020).
Google Scholar
Yu, J., Yaba, A., Kasiman, C., Thomson, T. & Johnson, J. mTOR controls ovarian follicle growth by regulating granulosa cell proliferation. PLoS ONE 6, e21415 (2011).
Google Scholar
Zhao, X. et al. The relationship between branched-chain amino acid related metabolomic signature and insulin resistance: a systematic review. J. Diabetes Res. 2016, 2794591 (2016).
Google Scholar
Lynch, C. J. & Adams, S. H. Branched-chain amino acids in metabolic signalling and insulin resistance. Nat. Rev. Endocrinol. 10, 723–736 (2014).
Google Scholar
Zhou, M. et al. Targeting BCAA catabolism to treat obesity-associated insulin resistance. Diabetes 68, 1730–1746 (2019).
Google Scholar
Tong, C., Wu, Y., Zhang, L. & Yu, Y. Insulin resistance, autophagy and apoptosis in patients with polycystic ovary syndrome: association with PI3K signaling pathway. Front. Endocrinol. 13, 1091147 (2022).
Google Scholar
Zhao, Y. et al. Up-regulated expression of WNT5a increases inflammation and oxidative stress via PI3K/AKT/NF-κB signaling in the granulosa cells of PCOS patients. J. Clin. Endocrinol. Metab. 100, 201–211 (2015).
Google Scholar
Li, D. et al. Autophagy is activated in the ovarian tissue of polycystic ovary syndrome. Reproduction 155, 85–92 (2018).
Google Scholar
Choi, J., Jo, M., Lee, E. & Choi, D. AKT is involved in granulosa cell autophagy regulation via mTOR signaling during rat follicular development and atresia. Reproduction 147, 73–80 (2014).
Google Scholar
Liu, M., Zhu, H., Zhu, Y. & Hu, X. Guizhi Fuling Wan reduces autophagy of granulosa cell in rats with polycystic ovary syndrome via restoring the PI3K/AKT/mTOR signaling pathway. J. Ethnopharmacol. 270, 113821 (2021).
Google Scholar
Ervin, S. M. et al. Gut microbial β-glucuronidases reactivate estrogens as components of the estrobolome that reactivate estrogens. J. Biol. Chem. 294, 18586–18599 (2019).
Google Scholar
Komorowski, A. S. & Pezo, R. C. Untapped “-omics”: the microbial metagenome, estrobolome, and their influence on the development of breast cancer and response to treatment. Breast Cancer Res. Treat. 179, 287–300 (2020).
Google Scholar
Liu, S. M. et al. Factors associated with effectiveness of treatment and reproductive outcomes in patients with thin endometrium undergoing estrogen treatment. Chin. Med. J. 128, 3173–3177 (2015).
Google Scholar
Marquardt, R. M., Kim, T. H., Shin, J. H. & Jeong, J. W. Progesterone and estrogen signaling in the endometrium: what goes wrong in endometriosis? Int. J. Mol. Sci. 20, (2019).
Fernandez-Fernandez, R., Aguilar, E., Tena-Sempere, M. & Pinilla, L. Effects of polypeptide YY(3-36) upon luteinizing hormone-releasing hormone and gonadotropin secretion in prepubertal rats: in vivo and in vitro studies. Endocrinology 146, 1403–1410 (2005).
Google Scholar
Gosman, G. G., Katcher, H. I. & Legro, R. S. Obesity and the role of gut and adipose hormones in female reproduction. Hum. Reprod. Update 12, 585–601 (2006).
Google Scholar
Ostadmohammadi, V., Jamilian, M., Bahmani, F. & Asemi, Z. Vitamin D and probiotic co-supplementation affects mental health, hormonal, inflammatory and oxidative stress parameters in women with polycystic ovary syndrome. J. Ovarian Res. 12, 5 (2019).
Google Scholar
Larraufie, P. et al. SCFAs strongly stimulate PYY production in human enteroendocrine cells. Sci. Rep. 8, 74 (2018).
Google Scholar
Pinilla, L. et al. Stimulatory effect of PYY-(3-36) on gonadotropin secretion is potentiated in fasted rats. Am. J. Physiol. Endocrinol. Metab. 290, E1162–E1171 (2006).
Google Scholar
Ehrström, S. et al. Lactic acid bacteria colonization and clinical outcome after probiotic supplementation in conventionally treated bacterial vaginosis and vulvovaginal candidiasis. Microbes Infect. 12, 691–699 (2010).
Google Scholar
Mändar et al. Impact of Lactobacillus crispatus-containing oral and vaginal probiotics on vaginal health: a randomised double-blind placebo controlled clinical trial. Benef. Microbes 14, 143–152 (2023).
Google Scholar
van de Wijgert, J. & Verwijs, M. C. Lactobacilli-containing vaginal probiotics to cure or prevent bacterial or fungal vaginal dysbiosis: a systematic review and recommendations for future trial designs. BJOG 127, 287–299 (2020).
Google Scholar
Cohen, C. R. et al. Randomized trial of lactin-V to prevent recurrence of bacterial vaginosis. N. Engl. J. Med. 382, 1906–1915 (2020).
Google Scholar
Adebola, O. O., Corcoran, O. & Morgan, W. A. Synbiotics: the impact of potential prebiotics inulin, lactulose and lactobionic acid on the survival and growth of lactobacilli probiotics. J. Funct. Food 10, 75–84 (2014).
Google Scholar
Bommasamudram, J., Muthu, A. & Devappa, S. Effect of prebiotics on thermally acclimatized lactobacilli cultures and their application as synbiotics in RTD fruit drinks. 3 Biotech 13, 311 (2023).
Google Scholar
Mitra, A. et al. Genital tract microbiota composition profiles and use of prebiotics and probiotics in gynaecological cancer prevention: review of the current evidence, the European Society of Gynaecological Oncology prevention committee statement. Lancet Microbe 5, e291–e300 (2024).
Google Scholar
Coste, I., Judlin, P., Lepargneur, J. P. & Bou-Antoun, S. Safety and efficacy of an intravaginal prebiotic gel in the prevention of recurrent bacterial vaginosis: a randomized double-blind study. Obstet. Gynecol. Int. 2012, 147867 (2012).
Google Scholar
Criscuolo, A. A. et al. Therapeutic efficacy of a Coriolus versicolor-based vaginal gel in women with cervical uterine high-risk HPV infection: a retrospective observational study. Adv. Ther. 38, 1202–1211 (2021).
Google Scholar
Lavitola, G., Della Corte, L., De Rosa, N., Nappi, C. & Bifulco, G. Effects on vaginal microbiota restoration and cervical epithelialization in positive HPV patients undergoing vaginal treatment with carboxy-methyl-beta-glucan. Biomed. Res. Int. 2020, 5476389 (2020).
Google Scholar
Serrano, L. et al. Efficacy of a Coriolus versicolor–based vaginal gel in women with human papillomavirus–dependent cervical lesions: the PALOMA study. J. Low. Genit. Tract. Dis. 25, 130–136 (2021).
Google Scholar
Stentella, P. et al. Efficacy of carboxymethyl beta-glucan in cervical intraepithelial neoplasia: a retrospective, case-control study. Minerva Ginecol. 69, 425–430 (2017).
Google Scholar
Gil-Antuñano, S. P. et al. Efficacy of a Coriolus versicolor-based vaginal gel in human papillomavirus-positive women older than 40 years: a sub-analysis of PALOMA study. J. Pers. Med. 12, 1559 (2022).
Google Scholar
Ma, D., Chen, Y. & Chen, T. Vaginal microbiota transplantation for the treatment of bacterial vaginosis: a conceptual analysis. FEMS Microbiol. Lett. 366, fnz025 (2019).
Google Scholar
Luo, H., Zhou, C., Zhou, L., He, Y. & Xie, R. H. The effectiveness of vaginal microbiota transplantation for vaginal dysbiosis and bacterial vaginosis: a scoping review. Arch. Gynecol. Obstet. 310, 643–653 (2024).
Google Scholar
Flores-Treviño, S. et al. Microbiota transplantation and administration of live biotherapeutic products for the treatment of dysbiosis-associated diseases. Expert Opin. Biol. Ther. 25, 1–14 (2025).
Google Scholar
Zhang, Z. et al. Human papillomavirus and cervical cancer in the microbial world: exploring the vaginal microecology. Front. Cell Infect. Microbiol. 14, 1325500 (2024).
Google Scholar
Wang, Y., Liu, Z. & Chen, T. Vaginal microbiota: potential targets for vulvovaginal candidiasis infection. Heliyon 10, e27239 (2024).
Google Scholar
Zhao, X., Liu, Z. & Chen, T. Potential role of vaginal microbiota in ovarian cancer carcinogenesis, progression and treatment. Pharmaceutics 15, 948 (2023).
Google Scholar
Lev-Sagie, A. et al. Vaginal microbiome transplantation in women with intractable bacterial vaginosis. Nat. Med. 25, 1500–1504 (2019).
Google Scholar
Wrønding, T. et al. Antibiotic-free vaginal microbiota transplant with donor engraftment, dysbiosis resolution and live birth after recurrent pregnancy loss: a proof of concept case study. EClinicalMedicine 61, (2023).
Rezazadeh, M. B., Zanganeh, M., Jarahi, L. & Fatehi, Z. Comparative efficacy of oral and vaginal probiotics in reducing the recurrence of bacterial vaginosis: a double-blind clinical trial. BMC Women’s Health 24, 575 (2024).
Google Scholar
Zhang, Y. et al. Probiotic Lacticaseibacillus rhamnosus GR-1 and Limosilactobacillus reuteri RC-14 as an adjunctive treatment for bacterial vaginosis do not increase the cure rate in a Chinese cohort: a prospective, parallel-group, randomized, controlled study. Front. Cell Infect. Microbiol. 11, 669901 (2021).
Google Scholar
Filardo, S., Di Pietro, M., Mastromarino, P., Porpora, M. G. & Sessa, R. A Multi-strain oral probiotic improves the balance of the vaginal microbiota in women with asymptomatic bacterial vaginosis: preliminary evidence. Nutrients 16, (2024).
Karamali, M. et al. The effects of synbiotic supplementation on pregnancy outcomes in gestational diabetes. Probiotics Antimicrob. Proteins 10, 496–503 (2018).
Google Scholar
Nachum, Z. et al. Oral probiotics to prevent recurrent vulvovaginal infections during pregnancy-multicenter double-blind, randomized, placebo-controlled trial. Nutrients 17, (2025).
Nulens, K. et al. Synbiotics in patients at risk for spontaneous preterm birth: protocol for a multi-centre, double-blind, randomised placebo-controlled trial (PRIORI). Trials 25, 615 (2024).
Google Scholar
Wu, S., Hugerth, L. W., Schuppe-Koistinen, I. & Du, J. The right bug in the right place: opportunities for bacterial vaginosis treatment. NPJ Biofilms Microbiomes 8, 34 (2022).
Google Scholar
Shoaei, T. et al. Effects of probiotic supplementation on pancreatic β-cell function and C-reactive protein in women with polycystic ovary syndrome: a randomized double-blind placebo-controlled clinical trial. Int. J. Prevent. Med. 6, 27 (2015).
Google Scholar
Rashad, N. M., Amal, S., Amin, A. I. & Soliman, M. H. Effects of probiotics supplementation on macrophage migration inhibitory factor and clinical laboratory feature of polycystic ovary syndrome. J. Funct. Food 36, 317–324 (2017).
Google Scholar
Heshmati, J. et al. The effects of probiotics or synbiotics supplementation in women with polycystic ovarian syndrome: a systematic review and meta-analysis of randomized clinical trials. Probiotics Antimicrob. Proteins 11, 1236–1247 (2019).
Google Scholar
Ghanei, N. et al. The probiotic supplementation reduced inflammation in polycystic ovary syndrome: a randomized, double-blind, placebo-controlled trial. J. Funct. Food 42, 306–311 (2018).
Google Scholar
Li, Y., Tan, Y., Xia, G. & Shuai, J. Effects of probiotics, prebiotics, and synbiotics on polycystic ovary syndrome: a systematic review and meta-analysis. Crit. Rev. Food Sci. Nutr. 63, 522–538 (2023).
Google Scholar
Angoorani, P. et al. The effects of probiotics, prebiotics, and synbiotics on polycystic ovarian syndrome: an overview of systematic reviews. Front. Med. 10, 1141355 (2023).
Google Scholar
Shamasbi, S. G., Ghanbari-Homayi, S. & Mirghafourvand, M. The effect of probiotics, prebiotics, and synbiotics on hormonal and inflammatory indices in women with polycystic ovary syndrome: a systematic review and meta-analysis. Eur. J. Nutr. 59, 433–450 (2020).
Google Scholar
link






