
Intervention development models
The study employed two complementary theoretical frameworks to guide the development of the intervention framework. First, the COM-B model from the Behaviour Change Wheel (BCW) provided the foundation for understanding behaviour change, informing the selection of behaviour change techniques, intervention functions, policy categories, and eventually, the strategies and delivery options. Second, Campinha-Bacote’s model of cultural competence in healthcare delivery supported the integration of cultural competence into the intervention design.These models were chosen over others because, while the BCW provides a standardised taxonomy to link outcomes with mechanisms of change, facilitating evaluation, replication, and comparison of interventions [13, 14]. The Campinha-Bacote model was adopted for its multidimensional view of cultural competence as a dynamic, ongoing process rather than a fixed skill set [15]. Together, these models were used to analyse the selected target behaviours within their specific context and to identify the precise changes required to achieve the desired behavioural outcomes.
Behaviour change wheel (BCW)
The Behaviour Change Wheel (BCW) is an intervention development method linked to a model of behaviour. It was developed from a synthesis of nineteen frameworks of behaviour change and has three layers (see Fig. 1). The COM-B model, which stands for capability (C), opportunity (O), motivation (M), and behaviour (B), is the hub for identifying the sources of behaviour to target in an intervention. For a behaviour to occur, individuals must have the capability, opportunity, and motivation. The second layer presents intervention functions, and the third layer presents potential policy options. The intervention functions and policy options provide a wide choice, allowing developers to consider the potential of each option. Using these as a guide, intervention developers choose the appropriate intervention function and policy option using the APEASE Criteria. APEASE includes six criteria (affordability, practicability, effectiveness/cost-effectiveness, acceptability, side effects/safety, and equity) against which each option is appraised, and those meeting all APEASE criteria should be considered.
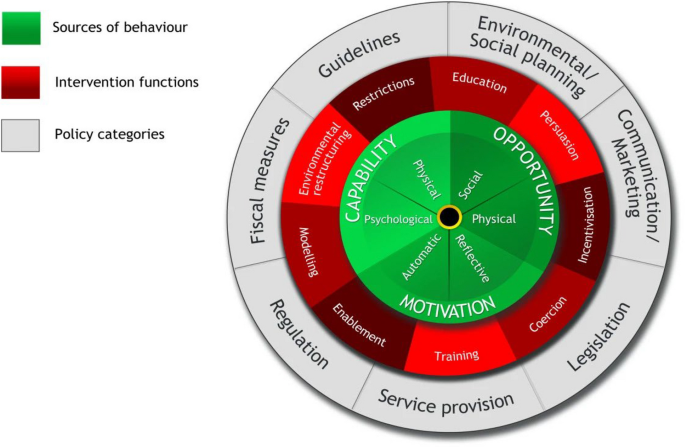
Behaviour change wheel. Source: Adopted from Michie et al., [36]
Campinha-bacote model of cultural competence in healthcare delivery
The growing diversity of global populations has compelled healthcare providers to prioritise cultural competence a continuous process of improving the ability to deliver equitable care across cultural boundaries [15, 16]. Campinha-Bacote’s model of culturally competent healthcare outlines five interrelated components: Cultural awareness involves self-reflection on personal biases and recognition of the power dynamics and privilege associated with the healthcare provider’s role [17]. Cultural skill refers to the ability to conduct sensitive, respectful, and thorough cultural assessments, grounded in humility and open-mindedness [18]. Cultural knowledge requires actively learning about the beliefs, health practices, and values of diverse populations while avoiding stereotypes and acknowledging variation within cultural groups [19]. Cultural encounter entails direct engagement with individuals from diverse backgrounds to challenge preconceptions and promote continuous learning [17, 20]. Cultural desire reflects the sincere and ongoing motivation to become culturally competent and to meaningfully engage in cross-cultural care [17]. These two theoretical frameworks guided the development of the intervention. The flow diagram below illustrates the process of developing the behaviour change intervention framework (see Fig. 2).
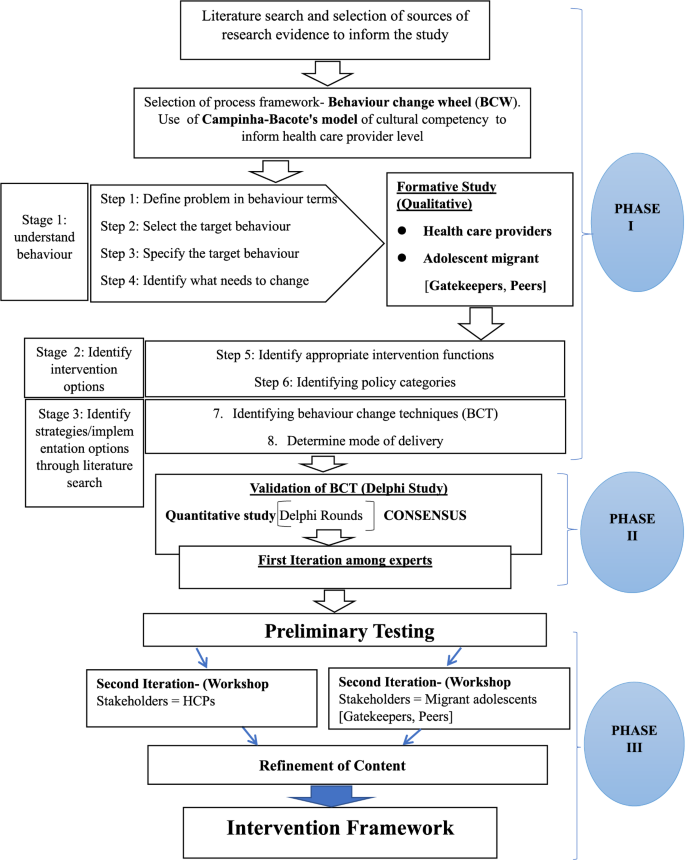
Flow diagram for behaviour change intervention framework development
Study sites
The study involves the use of a multi-study site in the Greater Accra Region including (a) Ussher hospital (Old Fadama), (b) Mallamata Government Hospital (Mallamata market and environs), (c)Madina Polyclinic-Kekele, Pentecost Hospital, Madina (Madina). These facilities were selected because they are used by migrant adolescents and are located within the catchment areas where these migrants live, largely due to strong migrant networks [21, 22].
Study design
The study adopted an intervention development design, incorporating multiple research methods to gather relevant and comprehensive information [23]. By combining both qualitative and quantitative approaches, the study aimed to either clarify findings from one method or enhance the depth and breadth of understanding [24, 25] .
Phase one: formative study and stakeholder engagement
Aim
To conduct an in-depth analysis of the behaviours to be changed, as a result identifying barriers and facilitators to enhance uptake of sexual and reproductive health service utilisation as well as delivery of services among health care professionals.
Study approach
The study adopts the phenomenology of qualitative research strategies. A phenomenological study explores what people experience and focuses on their experience of a phenomenon [26,27,28,29,30]. Therefore, collecting detailed information is necessary in order to understand and interpret the personal experiences of both migrant adolescents and HCPs in their interactions regarding the utilisation and delivery of ASRHs.
Population/sample size/sampling technique
The study was conducted among HCPs; midwives, nurses, community health nurses, and public health nurses, who operate within adolescent sexual and reproductive health clinics as well as migrant adolescents, peers, and their gatekeepers. Thirty-six (36) participants were initially selected to participate in the study, however due to saturation, when new themes no longer emerged [31], twenty-five (25) participants were used for the study. Data saturation was confirmed after three consecutive interviews yielded no new information [32]. The criterion sampling technique was used purposively to identify the healthcare facilities, and then convenience sampling technique was further used to select both the HCPs attending to clinical cases with the migrant adolescents. After identifying the migrant adolescents, a snowball sampling technique was employed to select their gatekeepers/guardians [33,34,35]. A snowball sampling technique was also employed to recruit peers of migrant adolescents in their various informal settlements.
Data collection method
A total of ten (10) in-depth interviews (IDI) were conducted among the migrant adolescents.
For the health care professionals, eight (8) interviews were conducted in all, which included; two (2) in-depth interviews (IDI), four (4) key informant interviews (KII), and two (2) focus group discussions (FGD) were held. In addition, three (3) key informant interviews (KII) were also held among the migrant’s gatekeepers, as well as four (4) in-depth interviews (IDI) for the migrant’s peers. The study spanned for 7 months.
Ethical clearance statement
The study received ethical approval from the Ghana Health Service Ethical Review Committee (Approval No. GHS-ERC 016/04/22), in accordance with the Declaration of Helsinki. Following approval, all participants including healthcare professionals, migrant adolescents, peers, gatekeepers, and Delphi panellists were fully informed about the study. Experts were contacted via email and confirmed their participation. Only individuals who provided written or thumb-printed consent were enrolled.
Voluntary Participation and Consent
Participation was voluntary, with the option to withdraw at any time without penalty. Written informed consent was obtained from all participants. For migrant adolescents aged 18–19, consent was obtained directly, while for those aged 10–17, guardian or gatekeeper permission and child assent were secured. Thumbprints were used for those unable to read or write.
Confidentiality
Data was anonymised using unique codes, and personal information was securely stored and accessible only to the principal investigator. No identifying information appeared in reports.
A description of stage 1 of the BCW
Stage 1: define the problem in behavioural terms
Steps 1–4 were undertaken at the formative stage involving the use of qualitative study as indicated above. This phase involved identification of what needs to change and how to change these outcomes [13]. In this study, the main problematic behaviour of public health concern that needed to be changed is poor utilisation of ASRHs among rural–urban migrant adolescents. To modify/change this behaviour, two important pathways; migrant adolescent’s behaviours (e.g. cultural norms, beliefs, trust, sense of entitlement, etc.) and HCPs behaviours (e.g. communication, self-efficacy, empathy, etc.) were hypothesized. HCP behaviours, for instance, are crucial, particularly when it comes to effectively communicating with migrant adolescents during clinical encounters, language barriers often pose a challenge in these interactions. This difficulty has the potential to negatively impact the sexual and reproductive health outcomes of adolescents. Therefore, to develop a comprehensive and effective intervention, it is crucial to simultaneously understand both demand-side behaviours (those of adolescents) and supply-side behaviours (those of HCPs), as poor uptake of ASRHs results from the interaction between these two dimensions.
Stage 2: identification of intervention options and policy categories to achieve the desired behaviour
In Step 5, intervention functions were identified as relevant based on the formative study findings, mapped onto the COM-B model. Using the Behaviour Change Wheel (BCW) framework [13], these functions were selected from the nine available options. The selection process also considered how well each function aligned with the targeted behaviours, the characteristics of the intended population, and the specific context in which the intervention would be implemented.
Step 6 of the Behaviour Change Wheel (BCW) framework involves identifying potential policy categories that could support the implementation of the intervention in real-world settings. Each intervention function identified in the previous step was mapped to relevant policy categories to determine which were most likely to be effective and appropriate. To guide the selection process, the APEASE criteria- Acceptability, Practicability, Effectiveness/cost-effectiveness, Affordability, Safety/side effects, and Equity- were applied to assess the suitability of each intervention function and policy category based on available evidence.
Stage 3: identification of implementation strategies and delivery options
Step 7 focused on identifying implementation strategies by selecting appropriate Behaviour Change Techniques (BCTs). BCTs have been defined as an observable, replicable, and irreducible component of an intervention designed to alter or redirect causal processes that regulate behaviour [36]. To identify appropriate BCTs, the same systematic approach used in previous steps was applied. The Behaviour Change Wheel (BCW) framework was used to Link each intervention function to recommended BCTs, ensuring that the strategies selected were evidence-based and contextually relevant. Together, these steps contributed to the development of a comprehensive intervention framework. For each intervention function, the most frequently and least frequently used BCTs are presented to guide users as a starting point for identifying BCTs Likely to be effective. For this study, the BCTs were assessed using the 93-item Behaviour Change Technique Taxonomy v1 [36]. Therefore, for each problematic behaviours and chosen intervention function(s) in the behavioural analysis, the appropriate BCTs were chosen by assessing the List of most and least frequent BCTs and the 93-item taxonomy at both the patient and provider level.To ensure the relevance and accuracy of the selected BCTs, a validation process was conducted using a Delphi study. Although a methodological approach was used to distil the problematic behaviours and map them to appropriate BCTs, validation was necessary to confirm the findings. This process involved input from both national and international experts in behaviour change interventions. Step 8 involved identifying the most suitable delivery methods for the intervention framework. This was achieved by determining which modes of delivery were relevant, practical, and feasible within the constraints of the setting and available resources.
Phase two: expert validation using the delphi method
Aim
To validate behaviour change technique taxonomies through expert input
Study methods/procedure
A quantitative research approach was adopted for this study. In September 2023, a letter of invitation was sent via email to potential experts, informing them about the study. A total of 130 national and international experts were initially approached oversampling to account for potential non-responses with the goal of obtaining at least 15 completed responses. Experts were selected based on their experience and knowledge in health behaviour change science and psychology. Of the experts invited, three declined participation due to unavailability. Ultimately, 10 experts provided complete responses, representing 66% of the targeted sample. While the final number was slightly below the anticipated 15, a sample of 10 is considered appropriate for a Delphi study. This aligns with findings in the Literature, where sample sizes typically range from 7 to 20 participants [37,38,39,40], and rarely exceed 30 [41]. Moreover, the appropriateness of this sample is further supported by the panel’s diversity in geographical representation and their substantial expertise in the subject area [42]. An expert sampling technique was initially used to purposively select participants based on their relevant expertise, followed by snowball sampling to select expert panel for the study. As part of the validation of the BCTs, consensus was reached using predefined decision rules to keep, delete, or modify the items. For this study, a consensus threshold of 70% agreement was applied, which is consistent with the standard practice in most Delphi studies, where thresholds typically range from 70 to 80% [43, 44]. Data were analysed using Stata version 16, employing descriptive statistics, including percentages of agreement, means, standard deviations, and ranges. Outcome measures included the appropriateness, feasibility, acceptability, and effectiveness of the Behaviour Change Techniques (BCTs). Additionally, the risk of harm was assessed by evaluating the Likelihood of BCTs causing harm or producing negative side effects for users or recipients of the intervention. This phase of the study lasted for 2months.
First iteration study
The first iteration, conducted in November 2023, involved re-engaging experts from the initial Delphi study.
Aim
To validate the accuracy of the implementation strategies and delivery modes derived from the BCTs. Their feedback was used to refine the intervention prototype.
Study procedure
The study employed quantitative descriptive design, aiming to quantify expert knowledge on the topic under discussion [45] (Cooper and Hedges, 1994). An email invitation was sent to the experts, informing them of the Delphi study outcomes and the proposed implementation strategies and delivery methods. A structured questionnaire, developed using Google Forms, was attached for completion.
The questions were based on key explanatory factors identified from both healthcare providers and adolescents, and were aligned with the Behaviour Change Techniques (BCTs), corresponding intervention strategies, and modes of delivery. The questionnaire included both closed- and open-ended questions, as well as Likert scale items rated on a 5-point scale: 1 = strongly agree, 2 = agree, 3 = neutral, 4 = disagree, and 5 = strongly disagree. The measures focused on perceived acceptability, appropriateness, and effectiveness of the proposed strategies. Data analysis involved univariate analysis using descriptive statistics, including the calculation of percentages for responses to the Likert scale items.
Phase three: preliminary testing of implementation strategies/mode of delivery—second iteration study and stakeholder engagement workshop
This phase involved engaging key users of the intervention, including healthcare providers (HCPs) and migrant adolescents.
Aim
To understand the extent to which the intervention aligns with the needs of key users, by identifying perceived barriers to implementation and suggesting alternative strategies to improve service uptake and delivery, while ensuring cultural relevance.
Study procedure
A qualitative research approach was employed for this study. The workshop included eight (8) healthcare professionals from all study sites, six (6) rural–urban migrant adolescents, three (3) peers, and two (2) gatekeepers. These participants had previously taken part in the formative study and met the eligibility criteria for inclusion. To accommodate HCPs availability, the workshop was held via Zoom, while migrant adolescents and other stakeholders attended in person.
Discussions were guided by a semi-structured instrument (Appendix III), adapted from Jenki et al. [46], focusing on potential barriers and alternative strategies for implementing the intervention and its delivery methods. The workshop lasted approximately 5–6 hours and included a breakout session. Outcome measures included acceptability; cultural appropriateness of the intervention for adolescents, peers, and gatekeepers, as well as feasibility; practical aspects of implementation from the perspective of healthcare providers. Workshop data were transcribed and uploaded to NVivo for thematic analysis. An inductive approach was used to identify themes and sub-themes based on the interview transcripts. A code book was developed to capture recurring patterns for reporting. The study was conducted in December 2024.
link






