
Health systems responsiveness (HSR) is one of the three intrinsic goals of health system performance, alongside health and fairness of financial contribution [1, 2]. Responsiveness relates to a health system’s ability to respond to the legitimate expectations of users about the non-medical aspects of care [3]. The concept of “health system responsiveness” is central to understanding people’s experiences of their health systems and how these experiences are shaped by the expectations of both service users and health system actors. In this way, peoples’ interactions with and evaluations of their health system is shaped by their initial expectations, as well as past experiences of care [1, 4]. HSR has a direct relationship with service utilisation, coverage and health outcomes (such as maternal mortality), service coverage, while also being influenced by financial protection coverage [1, 5]. HSR can also contribute to ensuring equity in access to quality care [6]. Routine HSR measurement is recommended for monitoring health system’s performance and the results can provide an opportunity for patient voices to be heard within the health care system [5]. This, in turn, can allow policymakers, practitioners, and researchers to anticipate and respond to patients’ existing and future health needs and expectations for better health outcomes.
The World Health Organization’s (WHO) original framework and conceptualisation of responsiveness has been well received by scholars and practitioners alike [7]. Within this conceptualisation, responsiveness is operationalised through the measurement of eight specific elements or domains: autonomy, choice of provider, confidentiality, communication, dignity, prompt attention, quality of basic amenities, and access to social support. The responsiveness of a health system is shaped by the expectations of individuals, families, and the broader community, as well as the health system’s capacity to respond to these expectations [6]. However, the characteristics of health services, peoples’ expectations, and the wider context has not yet received sufficient attention [4].
Mirzoev and Kane [4] proposed a conceptual framework that locates people’s experiences of interacting with their health system at the center of health system responsiveness. This framework includes the seven WHO domains and the additional domain of trust. These domains are important in determining people’s expectations and their decisions about whether to use health services. Two important determinants of people’s experiences of their interaction with health systems are people’s initial expectations (shaped by their characteristics and relationships within their families and communities) and the systems response to these expectations (e.g. through interactions with health providers who, in turn, also engage with policymakers and managers, as well as institutional and organisational arrangements, structures, and resources). In addition, the context (historical, political, cultural, and socioeconomic) is influential in shaping the interactions between the health system and people. Studies revealed that mental illness and medical treatment can undermine the dignity and autonomy of the patients [1] in which responsiveness is increasingly essential for such patients [8]. Health system responsiveness can involve both internal interactions amongst key health system actors, such as policymakers, managers, and providers, as well as external interactions between service users and health facility staff [4, 9]. Mirzoev and Kane’s [4] framework incorporates trust – interpersonal and institutional trust – as the eighth element of responsiveness. However, Valentine et al.’s [6] conceptualisation of responsiveness also acknowledges “clarity of communication” as an important feature of responsive health systems. Clarity of communication implies that providers clearly explain the nature of the illness to patients and their family, required treatment and treatment options, while also allowing sufficient time for patients to understand their symptoms and ask questions. As we explain further below, we incorporated Valentine et al.’s [6] notion of communication within the conceptual framework of responsiveness which guided our inquiry.
Health systems responsiveness has primarily been measured and examined using the corresponding WHO Multi Country Survey Study, structured around the eight domains of responsiveness. The tool asks respondents to rate their most recent encounter with the health system with respect to the eight elements of health systems responsiveness with Likert scale from 1–4 (1 being “very poor’ to 4 corresponding to ‘very good’). The health systems responsiveness questionnaire has been validated and applied in various country contexts, measuring the responsiveness of a range of health services. For instance, Liabsuetrakul et al. [10] examined the responsiveness of delivery care in Southern Thailand finding that women rated prompt attention, dignity, clear communication, and autonomy as particularly important aspects of care which ultimately influenced their choice of delivery facility. More broadly, Kapologwe et al. [11] assessed the responsiveness of primary care facilities in Tanzania finding that all domains of health system responsiveness were rated poorly except for confidentiality and dignity. Additional work by Awoke et al. [12] has highlighted the importance of examining the responsiveness of both public and private health services. In this study, respondents perceived that responsiveness was better in private, for-profit healthcare facilities, with higher wealth and multimorbidity being significant predictors of private healthcare utilisation. However, few studies have assessed health systems responsiveness at the primary care-level. However, some studies have compared health systems responsiveness between public and private providers. While studies have examined the responsiveness of mental health care in a high-income country context [8, 13], few have systematically examined the responsiveness of primary care towards the maternal and mental health needs of pregnant women in a low- and middle-income country context [10, 14].
Vietnam was among six countries that achieved the Millennium Development Goal-5 (MDG5) on reducing maternal mortality in 2015. The maternal mortality ratio (MMR) of the country has also declined considerably over time from 88 in 2000 to 46 in 2020 and is expected to reach the target of the National Action Plan to implement the 2030 Agenda. However, disparities in health outcomes and inequalities in maternal healthcare access and utilisation remain, especially for women from disadvantaged groups, such as those who are ethnic minorities [15]. Several factors can impact maternal mortality, including socioeconomic conditions, cultural and biological concerns, awareness of maternal health and psychological needs, insufficient health workforce numbers and skills, and limited access to maternal health services within the community. Poor maternal health outcomes are reported among women who have limited awareness of maternal health and psychological needs and those who lack access to skilled maternal health services [16]. The interaction of the mother with the healthcare system affects access, utilisation, coverage, as well as the well-being (health outcome) of the individual [10, 14, 17].
Studies from Vietnam have reported particularly high rates of common perinatal mental health disorders (CPMDs) in both rural and urban areas of the country. The prevalence rates of CPMDs, which refer to common mental disorders that occur during pregnancy or in the first year postpartum, range from 16.9%, to as high as 39.9% [18,19,20]. Multiple studies have highlighted the importance of paying attention to mental health in pregnancy due to the association between increased CPMD symptoms and intimate partner violence [21,22,23], as well as the normalisation of CPMDs during pregnancy [24] Despite the increasing burden of maternal mental health conditions, Vietnam’s mental health policy was last updated in 1989, with no community- or primary care-level policies addressing mental health [25]. Commune health centers (CHCs) are the first level of primary health care in Vietnam. However, while primary care workers at CHCs are intended to be the main gatekeepers to all mental health services, severe mental health conditions are treated at National and Provincial Psychiatric hospitals [23]. Moreover, there is currently no guidance, within the National Guideline on Reproductive Health Services (2009, 2016), on the screening for CPMDs within antenatal care. As a result, incidents of CPMDs, particularly in rural regions of Vietnam, can be largely overlooked [19]. Integration of maternal and mental health at the primary care-level could be one strategy for improving maternal mental health access and utilisation in Vietnam [26].
This study uses an adapted version of the Mirzoev and Kane [4] and Valentine et al. framework [6] on HSR to assess the responsiveness of the Vietnamese health system to pregnant women’s maternal and mental health needs (Fig. 1). Pregnant women with mental health needs should have to: (a) recognise their health needs, (b) decide to seek care, and then (c) initiate contact with the system/utilisation, and finally, (d) receive service coverage [6]. Care-seekers’ decisions related to utilisation of healthcare are influenced by three broad factors: (i) the personal context (family and friends, personal beliefs); (ii) providers (therapeutic guidelines/decisions, organisation of delivery, provider attitudes and reputation); and (iii) the perceived health system’s capacity to be responsive to peoples’ needs and expectations.
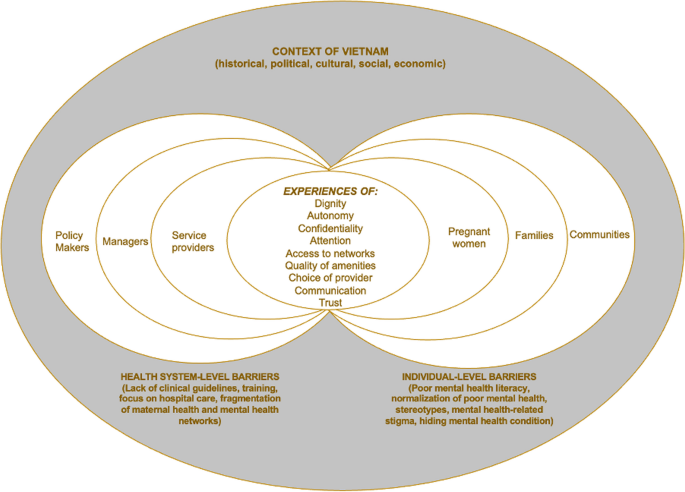
Conceptual framework on Health System Responsiveness in Vietnam. (Adapted from Mirzoev and Kane [4] and Valentine et al. framework [6])
The domains of health systems responsiveness comprise of nine domains covering the non-medical aspects of the interaction between people and their health systems. These domains progress from accessibility (users able to reach and use health services) and acceptability of care (users willing to use accessible services), and are influenced by individual- and system-level barriers.
At an individual-level, several barriers that have been identified in the literature include, poor mental health literacy, the normalisation of mental health or seeking alternative care for mental health, stereotypes of mental illness, a strong fear of mental health-related stigma, concealing one’s mental health condition, as well as self-treatment [24, 27]. Ultimately, these factors can lead to delays in seeking care.
At the health system-level, barriers can include, a lack of clinical guidelines on integrating mental health into routine ANC services and a lack of knowledge and training on mental health among maternal care providers [24, 27]. Other system-wide barriers may include applying a biomedical approach with a focus on hospital treatment of severe mental illness, and fragmented and siloed management and delivery of perinatal mental health [24, 27]. These barriers can lead to pervasive negative healthcare experiences and provider-patient relationships which can, in turn, prevent pregnant women from accessing mental health services. Pregnant women may avoid seeking mental health care altogether due to perceptions of poor treatment during the care encounter, low quality of existing services, or a lack of services in the first place [4, 6, 28]. Enhancing communication within the health system provides a potential entry point for improving responsiveness. Clear communication is associated with dignity, better involvement in decision-making, and, in addition, supports better coverage or access [6].
Previous studies on HSR have been published since 2000, but most of these focus on general health services, delivery care, and individual programmes such as mental health care. Very few have focused on intersecting health domains, such as pregnant women who have sought antenatal care services with mental health needs. Therefore, there is a knowledge gap about pregnant women’s perspectives on the responsiveness of ANC services. The main objective of this study is to assess pregnant women’s perceptions of the responsiveness of the Vietnamese health system to their mental health-related needs. We do so by utilising the WHO’s validated questionnaire on health systems responsiveness. We hope that our results will contribute towards strengthening the responsiveness of primary care in Vietnam to meet pregnant women’s mental health-related needs. We seek to define the measures needed to improve responsiveness which, in turn, can improve overall health system performance.
link






